Volume 22, Issue 1 (March 2024)
Iranian Rehabilitation Journal 2024, 22(1): 55-62 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Iqbal S F, Anwar N, Fatima A, Saqulain G. Effect of Slump Stretching and Straight Leg Raising Techniques for Lumbosacral Radiculopathy: A Comparative Study. Iranian Rehabilitation Journal 2024; 22 (1) :55-62
URL: http://irj.uswr.ac.ir/article-1-1810-en.html
URL: http://irj.uswr.ac.ir/article-1-1810-en.html
1- Department of Physical Therapy, Faculty of Allied Health Sciences, Riphah International University, Islamabad, Pakistan.
2- Department of Physical Therapy, Faculty of Allied Health Sciences, The University of Lahore, Lahore, Pakistan.
3- Department of Otorhinolaryngology, Capital Hospital Islamabad, Islamabad, Pakistan.
2- Department of Physical Therapy, Faculty of Allied Health Sciences, The University of Lahore, Lahore, Pakistan.
3- Department of Otorhinolaryngology, Capital Hospital Islamabad, Islamabad, Pakistan.
Full-Text [PDF 463 kb]
(1614 Downloads)
| Abstract (HTML) (2732 Views)
Full-Text: (636 Views)
Introduction
Low back pain (LBP) predominantly affects the musculoskeletal system causing disability. Lumbosacral radiculopathy is an important cause of LBP and is considered a syndrome with pain resulting from compression/irritation of nerve roots with radiation of pain to one or both lower extremities with the degree of spinal involvement specifying affected dermatome [1]. Radiculopathy involving the lumbar and sacral region is the compression involving the dorsal lumbar as well as sacral nerve roots. This leads to excruciating pain, numbness, and weak extremities. A sensation of tingling, numbness, and paresthesia may also be present [2]. The nerve roots exit the thecal sac in the lateral recess, hence, compression can occur in the thecal sac. This may result from problems like disc prolapse, bulge or hernia, hypertrophy of facet or ligament, spondylolisthesis, infection, and tumors [3].
With a lifetime prevalence of 60-85% for LBP [2], lumbar radiculopathy has an incidence of 4.86/100 persons-years [4] and an estimated prevalence of 3 to 5%, affecting men in their fourth and females in their fifth or sixth decade [3]. A literature gap exists as regards chronic LBP prevalence in developing nations. An Indian study reveals a prevalence of 23% for LBP with 30% having radicular pain [5]. The severity of radiculopathy may vary from mild with sensory changes, pain, and no motor loss; moderate with sensory changes or pain with mild loss of motor function; and severe when sensory symptoms and pain occur with marked motor loss which results in disability [6].
A variety of treatment options are available to treat lumbar radiculopathy and LBP. These include spinal surgery and medicines commonly used to control symptoms of pain with anti-inflammatories including both non-steroidal and steroidal with limited evidence in support. In addition, lumbar traction, and manual therapy are done by physiotherapists and chiropractors [1].
A variety of treatment methods are in use to treat LBP caused by lumbar radiculopathy by therapists including stretching and strengthening, interferential therapy, and manual or mechanical traction methods [7]. Literature reveals that manual therapy is quite effective in treating muscular diseases in cases with lumbar radiculopathy. Other physiotherapy recommendations include stimulation, electrotherapy, traction, taping, and exercises [8]. Improvement in cases with non-radicular LBP has also been reported, thus reducing the symptoms of short-term disability, pain, as well as symptom centralization [9]. Inadequate evidence is present to support the efficiency of slump stretching exercises in cases of patients presenting with LBP.
The straight leg raise (SLR) and slump tests are among the most common physical examination tests that are used for the assessment of LBP with the slump stretching technique (SST) being more sensitive than the SLR test [10]. However, findings contrary to this have been reported in another study [11]. Thus, previous literature holds contradictory views regarding the more accurate test of the two.
Since neurogenic LBР involves the distribution of the sciatic nerve, which is abnormally stimulated resulting in activation of signals [12]. This may be due to the sensitivity of the growing neural tissue suggesting the variability of neuro-dynamics. Ramos et al. in a study reported that the treatment with neural mobilization reduces the intensity of LBP and increases the lumbar mobility [13]. This can accelerate the process of recovery of the functional capacity and accelerate patients’ activities to normal daily life [14].
Slump stretching is a neuro-dynamic treatment and literature reveals low moderate levels of evidence in favor of the SST positively affecting pain in LBP cases [15]. Hence, the current study was designed to determine the impact of slump stretching and SLR therapy on pain, disability, and range of motion for cases suffering from lumbosacral radiculopathy. This study is important since it will better inform therapists regarding the two treatment modalities that were found effective in the literature.
Materials and Methods
The current randomized clinical trial recruited a sample of 26 cases with lumbosacral radiculopathy from Kanaan Physiotherapy Clinic, Lahore City, Pakistan. The sample included both genders, aged 30 to 50 years, having symptomatic lumbosacral radiculopathy or symptoms of provocation on SLR test at an angle of 45-70°, suffering pain sensation of mild or moderate degree ranging from 0-10 on numeric pain rating scale (NPRS), and pre-intervention modified Oswestry disability index (MODI) >10% [16]. Cases excluded included those presenting with red flags including sepsis, osteoporotic bones, fractures of the spine, previous surgery of the spine, pregnancy, cases incapable of holding an advisory position, recurring symptoms when the neck is flexed during the test, and those with SLR <45°. Also, cases suffering from lumbar spinal issues like stenosis, spondylolisthesis, spondylolysis, deformities, polyneuropathies of different etiology, ankylosing spondylitis, and those with systemic causes of LBP were excluded.
The study was conducted over a period of 9 months between 1 July 2021 to 31 March 2022. The sample size was calculated utilizing OpenEpi with a 5 % margin of error and 0.80 power of study [17]. A sample size of 26 was calculated assuming a 10% attrition rate.
Following the collection of basic demographic data including name, age, gender, height, weight, and body mass index (BMI), a thorough case history, full physical examination, and lumbar radiculopathy regional assessment was carried out by the main researcher, considering the selection criteria.
Tools used for data collection included a numeric rating scale (NPRS) to measure pain intensity, the MODI to determine how the back pain impacted patients to conduct daily life, and goniometer was used as an instrument to measure the available range of motion at the hip joint in active SLR.
Patients were equally divided into group A (SST) and group B (straight leg raising technique [SLRT]) using a lottery method. NPRS, MODI, and SLR range were noted both pre-intervention and post-intervention.
Group A (SST)
Slump stretching was conducted with the subject positioned sitting with feet on the wall. Overpressure was applied to flex the cervical spine and extend the knee to the extent that symptoms recurred. This position was maintained over 30 seconds with 3 to 5 times stretching in every session. Common treatment was also added with tibial nerve electrical stimulation applied for 10 mins in 4 sessions of exercises (lumber stabilization) for 4 days a week over 4 weeks. The complete treatment protocol extended for 16 sessions including 4 days a week for 4 weeks. The total length of each session was 25 to 30 mins [15].
Group B (SLRT)
In this technique, the subject was lying relaxed in a supine position with one pillow under the head. The affected limb was raised perpendicular to the surface in a standard SLR test until pain was felt in the back or until movement was restricted. The leg was brought a few degrees down and a series of gentle oscillations toward ankle dorsiflexion was instituted which mobilized the sciatic nerve. Gradually, the range was increased up to the maximum range of SLR until the symptom-free range was achieved. This position was held for about 30 seconds and 3 to 5 repetitions of stretches in every session of the patient. Common treatment was also added similar to that given for the slump treatment group [18].
Statistical analysis
The data analysis was done using SPSS software, version 21. With no significant difference between the groups, parametric tests were utilized including an independent sample t-test to measure differences between study groups, while a paired sample test was utilized for measuring within-group changes and P<0.05 was taken as significant.
Results
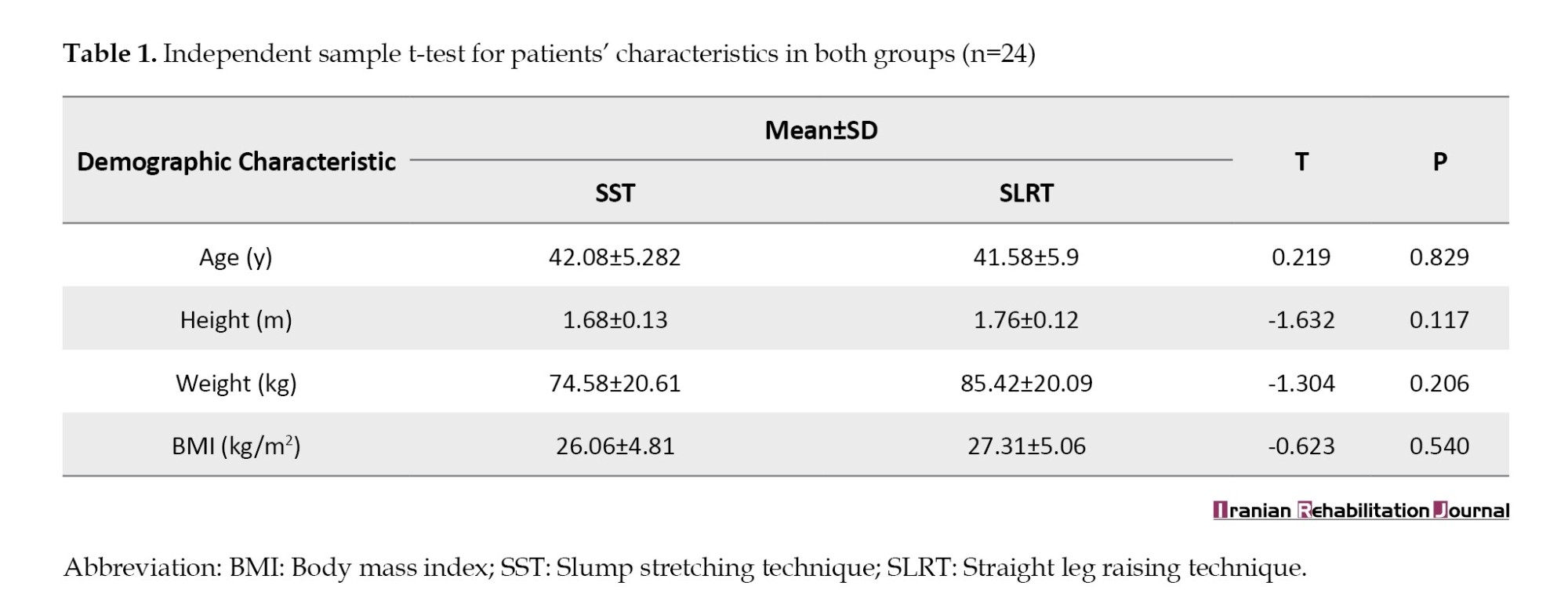
In the current research, twenty-six cases were physically screened between 1 July 2021 to 31 March 2022. Two patients withdrew from the study and 24 cases were randomized into the SST group (n=12) and SLRT group (n=12) group. This study revealed no significant difference between the SST group and SLRT group (P=0.829) with a mean age of 41.83±5.48 years and 42.08±5.28 years, respectively. No significant difference was noted for height (P=0.117), weight (P=0.206), and BMI (P=0.540) for both groups. The normality of data was determined utilizing the Shapiro-Wilk test. P>0.05 indicated that data was normally distributed, hence parametric tests were utilized for data analysis (Table 1).
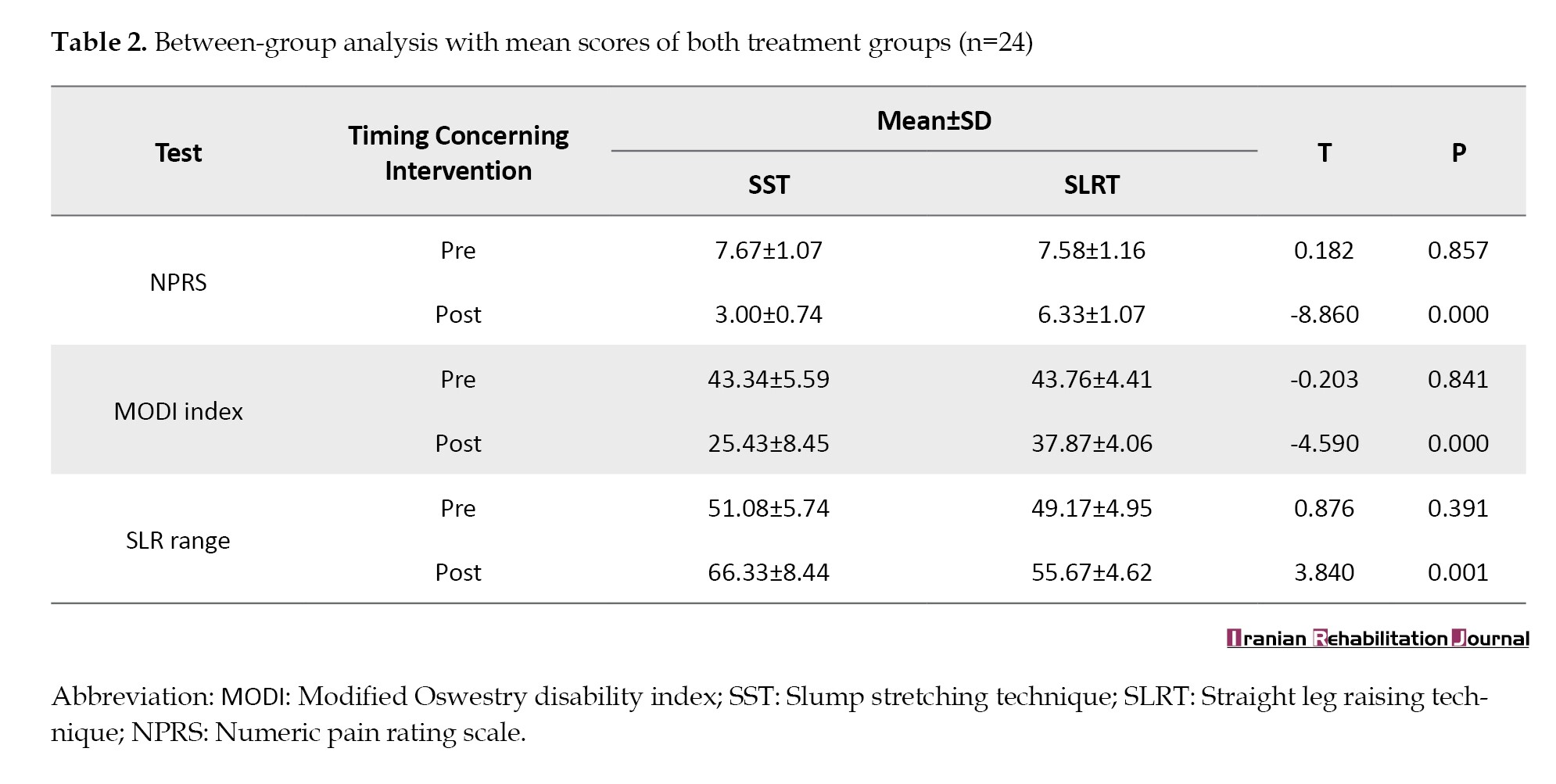
Between-group analysis (Table 2) revealed no significant difference before treatment between mean scores for SST and SLRT for NPRS (P=0.857), MODI (P=0.841), and SLR range (P=0.391). However, after receiving treatment, the mean scores for SST and SLRT revealed a significant difference for NPRS (P=0.000) with higher means for SLRT indicating more pain relief in SST, MODI (P=0.000) with higher scores for SLRT indicating SST showing greater improvement in disability, and SLR range (P=0.001) with higher scores for SST indicating increased range of motion.
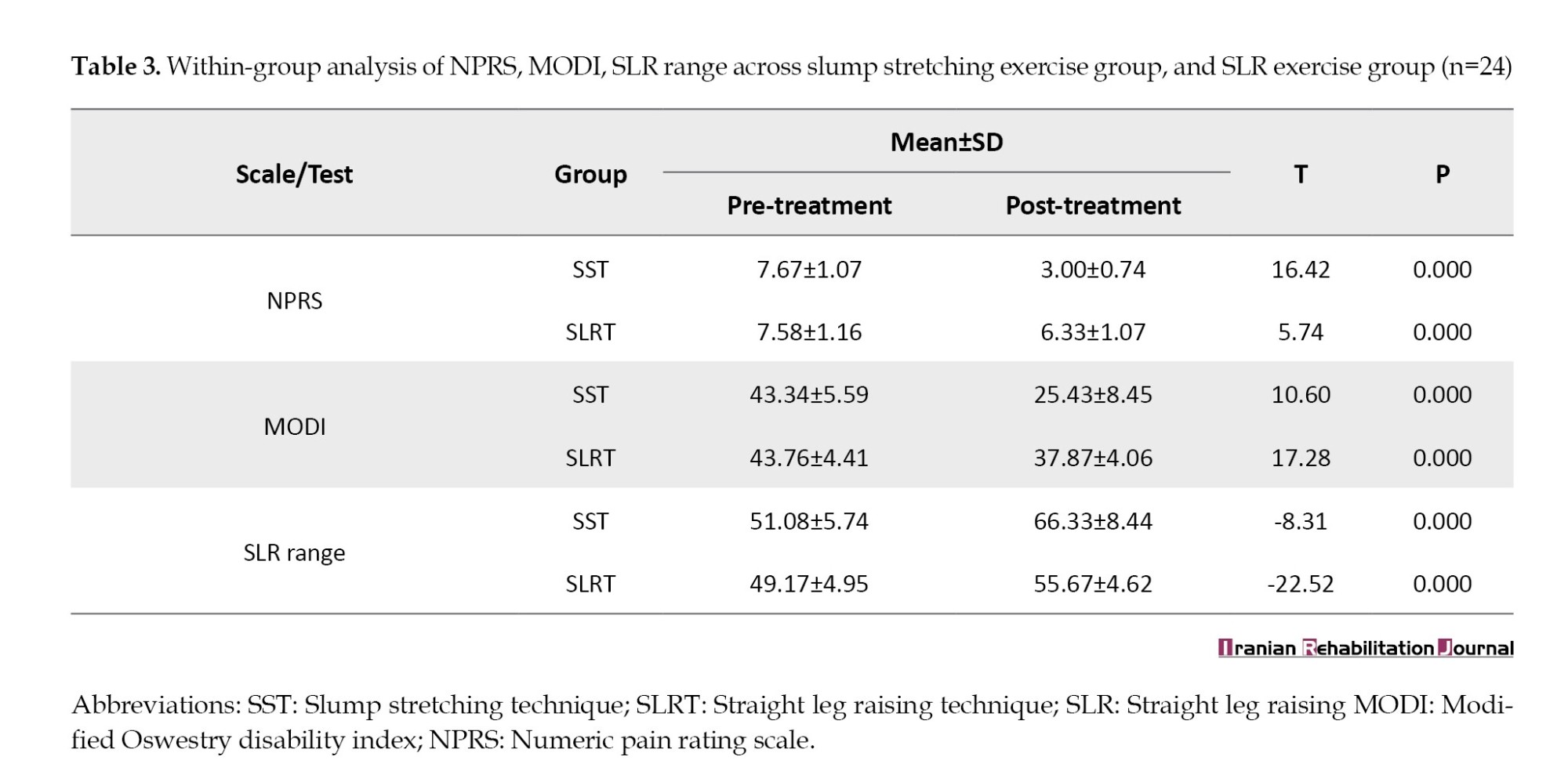
Within-group analysis revealed a significant difference (P<0.001) in both SST and SLRT groups, however, improvement was more pronounced for the SST group for NPRS, MODI, and SLR range (Table 3).
Discussion
The literature reveals the frequent use of SST for lumbosacral radiculopathy in a variety of non-homogenous populations [19]. This study compared the effect of the SLR technique and SST in patients with lumbosacral radiculopathy.
Study results revealed significantly (P<0.001) better post-treatment NPRS scores in the SST group with mean scores of 3.00±0.74 compared to 6.33±1.07 for the SLRT group. These results are in alignment with the study of Patel et al. which also showed that SST was better in treating pain as compared to SLRT [20]. SST is also effective in treating LBP presumably by decreasing intra-neural edema resulting in reduced neural tension and hypoalgesia mediated by C fibers [21]. In addition, inhibitory effects on the sympathetic system were also linked with SST since it also impacts the stretching capability of the nerve. Another reason that might explain pain reduction is that SST also results in decreasing adherence of scar tissue to neural tissue [21]. In contrast, Ferreira et al. reported no improvement in pain as well as disability with 15 days of neuro-dynamic management [22]. Similarly, in a study, Rezk-Allah SS et al. reported no significant difference in postoperative pain reduction between SST compared to SLRT in cases with herniation of lumbar disc [23]. These results contrast with the current study which revealed significantly better results for SST compared to the SLRT group through both revealed improvements. The SLRT group showed significant results in improving range following a previous study by Neal Hanney et al. who investigated the SLRT effects on hip flexion and found improvement in the range [24]. Similarly, SST also revealed significantly improved function compared to SLRT in a previous study involving lumbosacral radiculopathy [20]. However, the range of movement (ROM) results shown by SLRT were significantly better (P=0.001). Hence, SST was more effective for increasing the range with a mean score of 66.33±8.44 for the SST group compared to 55.66±4.61 for the SLRT group which complies with the results of the study by Mishra et al. [25]. A study by Adel revealed a significant reduction in pain, ROM, and nerve root compression post-neural mobilization compared to pre-mobilization due to neuro-dynamic stretch [26], which might explain this improvement in the range found in the current study. However, elastic deformation may also be the reason for this change [24]. The flexibility of the posterior myofascial chain is also affected by slump mobilization which causes an increase in the angle at the tibiotarsal joint and also increases finger-floor length. This can also act as a factor responsible for improving SLR values [27].
The current study used the MODI to measure the change in disability after applying treatment measures. Data analysis shows a significant (P<0.001) reduction in MODI in slump stretching pre-treatment from 43.34±5.59 to post-treatment 25.43±8.45 and SLR group pre-treatment (43.76±4.41) to post-treatment (37.87±4.06) indicating better results in slump group with more decrease in index score as compared to SLR group. These results are in agreement with a previous study which also compared these techniques in lumbar radiculopathy and showed similar results to the current study and proved SLRT less effective compared to SST [20]. Another study that investigated the effects of neuro-dynamic mobilization on radiculopathy of the lumbosacral region revealed that neuro-dynamic treatment along with conventional treatment enhanced the improvement in disability [2]. These results are in agreement with the current study in which both groups showed a significant decrease in MODI scores with P<0.001. This is also in agreement with the study by Bertolini et al. which reveals that demyelination is affected by pressure perceived by the nerve due to compression of micro-circulation, and these neuro-dynamic techniques help disperse the edema, thus causing a reduction in associated symptoms [28]. Additionally, neural mobilization can help reduce tension and friction resulting in a reduction of mechano-sensitivity [29]. Therefore, a neuro-dynamic method is a superior form of management when given in radiculopathy as it decreases pain and might be the reason for improved function in back pain due to radicular problems in the lumbosacral area. In contrast to the current study, Ferriera et al. reported that the score of disability index did not show any significant improvement in disability when analyzed at the interval of two weeks [22].
The results of this study suggested that the combined effect of the treatment program of lumbar stabilization and neural mobilization are very significant in LBP of radicular origin as shown by Gupta in his study. He found that Nerve mobilization techniques are effective in enhancing patient outcomes when applied in addition to standard care in managing sciatica [30]. Hence, this study proved that the SST group is more effective in improving pain, disability, and ROM.
Conclusion
This study concludes that however both slump stretching and SLRT result in improvement, the SST is significantly more effective than the SLRT in reducing pain, functional disability, and enhancing the range of SLR in cases suffering from lumbosacral radiculopathy.
Ethical Considerations
Compliance with ethical guidelines
This research approved by the Ethical Committee of Riphah International University (Code:# REC/RCR & AHS/21/0134). Written consent was obtained from all participants for inclusion in the study.
Funding
This article extracted from master's thesis of Sidra Firdous Iqbal, approved by Riphah International University.
Authors' contributions
Conceptualization: Arooj Fatima and Naveed Anwar; Methodology, resources and data curation: Sidra Firdous and Arooj Fatima; Formal analysis and writing the original draft: Naveed Anwar and Ghulam Saqulain; Review and editing: Ghulam Saqulain and Sidra Firdous; Supervision: All authors.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
The authors are indebted to administration of Kanaan Physiotherapy Clinic for making this study possible.
References
Low back pain (LBP) predominantly affects the musculoskeletal system causing disability. Lumbosacral radiculopathy is an important cause of LBP and is considered a syndrome with pain resulting from compression/irritation of nerve roots with radiation of pain to one or both lower extremities with the degree of spinal involvement specifying affected dermatome [1]. Radiculopathy involving the lumbar and sacral region is the compression involving the dorsal lumbar as well as sacral nerve roots. This leads to excruciating pain, numbness, and weak extremities. A sensation of tingling, numbness, and paresthesia may also be present [2]. The nerve roots exit the thecal sac in the lateral recess, hence, compression can occur in the thecal sac. This may result from problems like disc prolapse, bulge or hernia, hypertrophy of facet or ligament, spondylolisthesis, infection, and tumors [3].
With a lifetime prevalence of 60-85% for LBP [2], lumbar radiculopathy has an incidence of 4.86/100 persons-years [4] and an estimated prevalence of 3 to 5%, affecting men in their fourth and females in their fifth or sixth decade [3]. A literature gap exists as regards chronic LBP prevalence in developing nations. An Indian study reveals a prevalence of 23% for LBP with 30% having radicular pain [5]. The severity of radiculopathy may vary from mild with sensory changes, pain, and no motor loss; moderate with sensory changes or pain with mild loss of motor function; and severe when sensory symptoms and pain occur with marked motor loss which results in disability [6].
A variety of treatment options are available to treat lumbar radiculopathy and LBP. These include spinal surgery and medicines commonly used to control symptoms of pain with anti-inflammatories including both non-steroidal and steroidal with limited evidence in support. In addition, lumbar traction, and manual therapy are done by physiotherapists and chiropractors [1].
A variety of treatment methods are in use to treat LBP caused by lumbar radiculopathy by therapists including stretching and strengthening, interferential therapy, and manual or mechanical traction methods [7]. Literature reveals that manual therapy is quite effective in treating muscular diseases in cases with lumbar radiculopathy. Other physiotherapy recommendations include stimulation, electrotherapy, traction, taping, and exercises [8]. Improvement in cases with non-radicular LBP has also been reported, thus reducing the symptoms of short-term disability, pain, as well as symptom centralization [9]. Inadequate evidence is present to support the efficiency of slump stretching exercises in cases of patients presenting with LBP.
The straight leg raise (SLR) and slump tests are among the most common physical examination tests that are used for the assessment of LBP with the slump stretching technique (SST) being more sensitive than the SLR test [10]. However, findings contrary to this have been reported in another study [11]. Thus, previous literature holds contradictory views regarding the more accurate test of the two.
Since neurogenic LBР involves the distribution of the sciatic nerve, which is abnormally stimulated resulting in activation of signals [12]. This may be due to the sensitivity of the growing neural tissue suggesting the variability of neuro-dynamics. Ramos et al. in a study reported that the treatment with neural mobilization reduces the intensity of LBP and increases the lumbar mobility [13]. This can accelerate the process of recovery of the functional capacity and accelerate patients’ activities to normal daily life [14].
Slump stretching is a neuro-dynamic treatment and literature reveals low moderate levels of evidence in favor of the SST positively affecting pain in LBP cases [15]. Hence, the current study was designed to determine the impact of slump stretching and SLR therapy on pain, disability, and range of motion for cases suffering from lumbosacral radiculopathy. This study is important since it will better inform therapists regarding the two treatment modalities that were found effective in the literature.
Materials and Methods
The current randomized clinical trial recruited a sample of 26 cases with lumbosacral radiculopathy from Kanaan Physiotherapy Clinic, Lahore City, Pakistan. The sample included both genders, aged 30 to 50 years, having symptomatic lumbosacral radiculopathy or symptoms of provocation on SLR test at an angle of 45-70°, suffering pain sensation of mild or moderate degree ranging from 0-10 on numeric pain rating scale (NPRS), and pre-intervention modified Oswestry disability index (MODI) >10% [16]. Cases excluded included those presenting with red flags including sepsis, osteoporotic bones, fractures of the spine, previous surgery of the spine, pregnancy, cases incapable of holding an advisory position, recurring symptoms when the neck is flexed during the test, and those with SLR <45°. Also, cases suffering from lumbar spinal issues like stenosis, spondylolisthesis, spondylolysis, deformities, polyneuropathies of different etiology, ankylosing spondylitis, and those with systemic causes of LBP were excluded.
The study was conducted over a period of 9 months between 1 July 2021 to 31 March 2022. The sample size was calculated utilizing OpenEpi with a 5 % margin of error and 0.80 power of study [17]. A sample size of 26 was calculated assuming a 10% attrition rate.
Following the collection of basic demographic data including name, age, gender, height, weight, and body mass index (BMI), a thorough case history, full physical examination, and lumbar radiculopathy regional assessment was carried out by the main researcher, considering the selection criteria.
Tools used for data collection included a numeric rating scale (NPRS) to measure pain intensity, the MODI to determine how the back pain impacted patients to conduct daily life, and goniometer was used as an instrument to measure the available range of motion at the hip joint in active SLR.
Patients were equally divided into group A (SST) and group B (straight leg raising technique [SLRT]) using a lottery method. NPRS, MODI, and SLR range were noted both pre-intervention and post-intervention.
Group A (SST)
Slump stretching was conducted with the subject positioned sitting with feet on the wall. Overpressure was applied to flex the cervical spine and extend the knee to the extent that symptoms recurred. This position was maintained over 30 seconds with 3 to 5 times stretching in every session. Common treatment was also added with tibial nerve electrical stimulation applied for 10 mins in 4 sessions of exercises (lumber stabilization) for 4 days a week over 4 weeks. The complete treatment protocol extended for 16 sessions including 4 days a week for 4 weeks. The total length of each session was 25 to 30 mins [15].
Group B (SLRT)
In this technique, the subject was lying relaxed in a supine position with one pillow under the head. The affected limb was raised perpendicular to the surface in a standard SLR test until pain was felt in the back or until movement was restricted. The leg was brought a few degrees down and a series of gentle oscillations toward ankle dorsiflexion was instituted which mobilized the sciatic nerve. Gradually, the range was increased up to the maximum range of SLR until the symptom-free range was achieved. This position was held for about 30 seconds and 3 to 5 repetitions of stretches in every session of the patient. Common treatment was also added similar to that given for the slump treatment group [18].
Statistical analysis
The data analysis was done using SPSS software, version 21. With no significant difference between the groups, parametric tests were utilized including an independent sample t-test to measure differences between study groups, while a paired sample test was utilized for measuring within-group changes and P<0.05 was taken as significant.
Results
In the current research, twenty-six cases were physically screened between 1 July 2021 to 31 March 2022. Two patients withdrew from the study and 24 cases were randomized into the SST group (n=12) and SLRT group (n=12) group. This study revealed no significant difference between the SST group and SLRT group (P=0.829) with a mean age of 41.83±5.48 years and 42.08±5.28 years, respectively. No significant difference was noted for height (P=0.117), weight (P=0.206), and BMI (P=0.540) for both groups. The normality of data was determined utilizing the Shapiro-Wilk test. P>0.05 indicated that data was normally distributed, hence parametric tests were utilized for data analysis (Table 1).

Between-group analysis (Table 2) revealed no significant difference before treatment between mean scores for SST and SLRT for NPRS (P=0.857), MODI (P=0.841), and SLR range (P=0.391). However, after receiving treatment, the mean scores for SST and SLRT revealed a significant difference for NPRS (P=0.000) with higher means for SLRT indicating more pain relief in SST, MODI (P=0.000) with higher scores for SLRT indicating SST showing greater improvement in disability, and SLR range (P=0.001) with higher scores for SST indicating increased range of motion.

Within-group analysis revealed a significant difference (P<0.001) in both SST and SLRT groups, however, improvement was more pronounced for the SST group for NPRS, MODI, and SLR range (Table 3).

Discussion
The literature reveals the frequent use of SST for lumbosacral radiculopathy in a variety of non-homogenous populations [19]. This study compared the effect of the SLR technique and SST in patients with lumbosacral radiculopathy.
Study results revealed significantly (P<0.001) better post-treatment NPRS scores in the SST group with mean scores of 3.00±0.74 compared to 6.33±1.07 for the SLRT group. These results are in alignment with the study of Patel et al. which also showed that SST was better in treating pain as compared to SLRT [20]. SST is also effective in treating LBP presumably by decreasing intra-neural edema resulting in reduced neural tension and hypoalgesia mediated by C fibers [21]. In addition, inhibitory effects on the sympathetic system were also linked with SST since it also impacts the stretching capability of the nerve. Another reason that might explain pain reduction is that SST also results in decreasing adherence of scar tissue to neural tissue [21]. In contrast, Ferreira et al. reported no improvement in pain as well as disability with 15 days of neuro-dynamic management [22]. Similarly, in a study, Rezk-Allah SS et al. reported no significant difference in postoperative pain reduction between SST compared to SLRT in cases with herniation of lumbar disc [23]. These results contrast with the current study which revealed significantly better results for SST compared to the SLRT group through both revealed improvements. The SLRT group showed significant results in improving range following a previous study by Neal Hanney et al. who investigated the SLRT effects on hip flexion and found improvement in the range [24]. Similarly, SST also revealed significantly improved function compared to SLRT in a previous study involving lumbosacral radiculopathy [20]. However, the range of movement (ROM) results shown by SLRT were significantly better (P=0.001). Hence, SST was more effective for increasing the range with a mean score of 66.33±8.44 for the SST group compared to 55.66±4.61 for the SLRT group which complies with the results of the study by Mishra et al. [25]. A study by Adel revealed a significant reduction in pain, ROM, and nerve root compression post-neural mobilization compared to pre-mobilization due to neuro-dynamic stretch [26], which might explain this improvement in the range found in the current study. However, elastic deformation may also be the reason for this change [24]. The flexibility of the posterior myofascial chain is also affected by slump mobilization which causes an increase in the angle at the tibiotarsal joint and also increases finger-floor length. This can also act as a factor responsible for improving SLR values [27].
The current study used the MODI to measure the change in disability after applying treatment measures. Data analysis shows a significant (P<0.001) reduction in MODI in slump stretching pre-treatment from 43.34±5.59 to post-treatment 25.43±8.45 and SLR group pre-treatment (43.76±4.41) to post-treatment (37.87±4.06) indicating better results in slump group with more decrease in index score as compared to SLR group. These results are in agreement with a previous study which also compared these techniques in lumbar radiculopathy and showed similar results to the current study and proved SLRT less effective compared to SST [20]. Another study that investigated the effects of neuro-dynamic mobilization on radiculopathy of the lumbosacral region revealed that neuro-dynamic treatment along with conventional treatment enhanced the improvement in disability [2]. These results are in agreement with the current study in which both groups showed a significant decrease in MODI scores with P<0.001. This is also in agreement with the study by Bertolini et al. which reveals that demyelination is affected by pressure perceived by the nerve due to compression of micro-circulation, and these neuro-dynamic techniques help disperse the edema, thus causing a reduction in associated symptoms [28]. Additionally, neural mobilization can help reduce tension and friction resulting in a reduction of mechano-sensitivity [29]. Therefore, a neuro-dynamic method is a superior form of management when given in radiculopathy as it decreases pain and might be the reason for improved function in back pain due to radicular problems in the lumbosacral area. In contrast to the current study, Ferriera et al. reported that the score of disability index did not show any significant improvement in disability when analyzed at the interval of two weeks [22].
The results of this study suggested that the combined effect of the treatment program of lumbar stabilization and neural mobilization are very significant in LBP of radicular origin as shown by Gupta in his study. He found that Nerve mobilization techniques are effective in enhancing patient outcomes when applied in addition to standard care in managing sciatica [30]. Hence, this study proved that the SST group is more effective in improving pain, disability, and ROM.
Conclusion
This study concludes that however both slump stretching and SLRT result in improvement, the SST is significantly more effective than the SLRT in reducing pain, functional disability, and enhancing the range of SLR in cases suffering from lumbosacral radiculopathy.
Ethical Considerations
Compliance with ethical guidelines
This research approved by the Ethical Committee of Riphah International University (Code:# REC/RCR & AHS/21/0134). Written consent was obtained from all participants for inclusion in the study.
Funding
This article extracted from master's thesis of Sidra Firdous Iqbal, approved by Riphah International University.
Authors' contributions
Conceptualization: Arooj Fatima and Naveed Anwar; Methodology, resources and data curation: Sidra Firdous and Arooj Fatima; Formal analysis and writing the original draft: Naveed Anwar and Ghulam Saqulain; Review and editing: Ghulam Saqulain and Sidra Firdous; Supervision: All authors.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
The authors are indebted to administration of Kanaan Physiotherapy Clinic for making this study possible.
References
- Alexander CE, Varacallo M. Lumbosacral radiculopathy. Treasure Island: StatPearls Publishing; 2022. [Link]
- Sharma SS, Sheth MS. Effect of neurodynamic mobilization on pain and function in subjects with lumbosacral radiculopathy. Medicine Science. 2018; 7(1):5-8. [DOI:10.5455/medscience.2017.06.8664]
- Berry JA, Elia C, Saini HS, Miulli DE. A review of lumbar radiculopathy, diagnosis, and treatment. Cureus. 2019; 11(10):e5934. [DOI:10.7759/cureus.5934]
- Schoenfeld AJ, Laughlin M, Bader JO, Bono CM. Characterization of the incidence and risk factors for the development of lumbar radiculopathy. Journal of Spinal Disorders & Techniques. 2012; 25(3):163-7. [DOI:10.1097/BSD.0b013e3182146e55] [PMID]
- Paraseth TK, Gajendran M, James D. Approach to chronic low back pain in a rural mission hospital: An audit report. Chrismed: Journal of Health & Research. 2018; 5(1):43-7. [DOI:10.4103/cjhr.cjhr_40_17]
- Dydyk A, Khan MZ, Singh P. Radicular back pain. Treasure Island: StatPearls Publishing; 2021. [Link]
- Das S, Dowle P, Iyengar R. Effect of spinal mobilization with leg movement as an adjunct to neural mobilization and conventional therapy in patients with lumbar radiculopathy: Randomized controlled trial. Journal of Medical and Scientific Research. 2018; 6(1):11-9. [DOI:10.17727/JMSR.2018/6-3]
- Satpute K, Hall T, Bisen R, Lokhande P. The effect of spinal mobilization with leg movement in patients with lumbar radiculopathy-A double-blind randomized controlled trial. Archives of Physical Medicine and Rehabilitation. 2019; 100(5):828-36. [DOI:10.1016/j.apmr.2018.11.004] [PMID]
- Cleland JA, Childs JD, Palmer JA, Eberhart S. Slump stretching in the management of non-radicular low back pain: A pilot clinical trial. Manual Therapy. 2006; 11(4):279-86. [DOI:10.1016/j.math.2005.07.002] [PMID]
- Majlesi J, Togay H, Unalan H, Toprak S. The sensitivity and specificity of the slump and the straight leg raising tests in patients with lumbar disc herniation. Journal of Clinical Rheumatology. 2008; 14(2):87-91. [DOI:10.1097/RHU.0b013e31816b2f99] [PMID]
- M'kumbuzi VR, Ntawukuriryayo JT, Haminana JD, Munyandamutsa J, Nzakizwanimana E. Accuracy of straight leg raise and slump tests in detecting lumbar disc herniation: A pilot study. The Central African Journal of Medicine. 2012; 58(1-4):5-11. [PMID]
- Wong CE, Hu CY, Lee PH, Huang CC, Huang HW, Huang CY, et al. Sciatic nerve stimulation alleviates acute neuropathic pain via modulation of neuroinflammation and descending pain inhibition in a rodent model. Journal of Neuroinflammation. 2022; 19(1):153. [DOI:10.1186/s12974-022-02513-y] [PMID] [PMCID]
- Ramos M, Cruz CAH, Laurentino MF, Ashmawi HA, Santos FM, Chacur M. Effects of neural mobilization on individuals with chronic low back pain. Brazilian Journal of Pain. 2020; 3(3):205-12. [DOI:10.5935/2595-0118.20200041]
- Efstathiou MA, Stefanakis M, Savva C, Giakas G. Effectiveness of neural mobilization in patients with spinal radiculopathy: A critical review. Journal of Bodywork and Movement Therapies. 2015; 19(2):205-12. [DOI:10.1016/j.jbmt.2014.08.006] [PMID]
- Pourahmadi M, Hesarikia H, Keshtkar A, Zamani H, Bagheri R, Ghanjal A, et al. Effectiveness of slump stretching on low back pain: A systematic review and meta-analysis. Pain Medicine. 2019; 20(2):378-96. [DOI:10.1093/pm/pny208] [PMID]
- Fritz JM, Irrgang JJ. A comparison of a modified oswestry low back pain disability questionnaire and the quebec back pain disability scale. Physical Therapy. 2001; 81(2):776-88. [DOI:10.1093/ptj/81.2.776] [PMID]
- Sapra RL. How to calculate an adequate sample size? In: Nundy S, Kakar A, Bhutta ZA, editors. How to practice academic medicine and publish from developing countries? New York: Springer; 2022. [DOI:10.1007/978-981-16-5248-6_9]
- Willhuber GOC, Piuzzi NS. Straight leg raise test. Treasure Island: StatPearls Publishing; 2022. [Link]
- Nagrale AV, Patil SP, Gandhi RA, Learman K. Effect of slump stretching versus lumbar mobilization with exercise in subjects with non-radicular low back pain: A randomized clinical trial. The Journal of Manual & Manipulative Therapy. 2012; 20(1):35-42. [DOI:10.1179/2042618611Y.0000000015] [PMID] [PMCID]
- Patel N, Sharma S. A comparative study on effects of two different techniques of neural tissue mobilization in subjects with lumbosacral radiculopathy. International Journal of Physiology, Nutrition and Physical Education. 2018; 3(2):91-5. [Link]
- Beneciuk JM, Bishop MD, George SZ. Effects of upper extremity neural mobilization on thermal pain sensitivity: A sham-controlled study in asymptomatic participants. The Journal of Orthopaedic and Sports Physical Therapy. 2009; 39(6):428-38. [DOI:10.2519/jospt.2009.2954] [PMID]
- Ferreira G, Stieven F, Araujo F, Wiebusch M, Rosa C, Plentz R, et al. Neurodynamic treatment did not improve pain and disability at two weeks in patients with chronic nerve-related leg pain: A randomised trial. Journal of Physiotherapy. 2016; 62(4):197-202. [DOI:10.1016/j.jphys.2016.08.007] [PMID]
- Rezk-Allah SS, Shehata LA, Gharib NM. Slump stretching versus straight leg raising in the management of lumbar disc herniation. Egyptian Journal of Neurology, Psychiatry & Neurosurgery. 2011; 48(4):345-9. [Link]
- Neal Hanney R, Ridehalgh C, Dawson A, Lewis D, Kenny D. The effects of neurodynamic straight leg raise treatment duration on range of hip flexion and protective muscle activity at P1. Journal of Manual & Manipulative Therapy. 2016; 24(1):14-20. [DOI:10.1179/2042618613Y.0000000049] [PMID] [PMCID]
- Mishra S, Sarfare B, Ghodey S. Comparison between mulligan traction leg raise versus slumps stretching on pain, passive leg raise, and functional disability in lumbar radiculopathy. Journal of Medical Science and Clinical Research. 2018; 6(6):140-6. [DOI:10.18535/jmscr/v6i6.24]
- Adel SM. Efficacy of neural mobilization in treatment of low back dysfunctions. Journal of American Science. 2011; 7(4):566-73. [Link]
- Sharma S, Verma SK, Agarwal V. Effects of Neural Mobilization in Posterior Myofacial Chain Flexibility in Normal Subjects. Int J Physiother Res 2015;3(4):1122-25. [DOI:.10.16965/ijpr.2015.140]
- Bertolini GR, Silva TS, Trindade DL, Ciena AP, Carvalho AR. Neural mobilization and static stretching in an experimental sciatica model: An experimental study. Brazilian Journal of Physical Therapy. 2009; 13(6):493-8. [DOI:10.1590/S1413-35552009005000062]
- Neto T, Freitas SR, Andrade RJ, Gomes J, Vaz J, Mendes B, et al. Sciatic nerve stiffness is not changed immediately after a slump neurodynamics technique. Muscles, Ligaments and Tendons Journal. 2018; 7(3):583-9. [DOI:10.11138/mltj/2017.7.3.583] [PMID] [PMCID]
- Gupta M. Effectiveness of nerve mobilization in the management of sciatica. Indian Journal of Physiotherapy and Occupational Therapy. 2012; 6(2):79-81. [Link]
Article type: Original Research Articles |
Subject:
methodology in rehabilitation
Received: 2022/11/5 | Accepted: 2023/10/11 | Published: 2024/03/1
Received: 2022/11/5 | Accepted: 2023/10/11 | Published: 2024/03/1
Send email to the article author








