Volume 23, Issue 3 (September 2025)
Iranian Rehabilitation Journal 2025, 23(3): 247-256 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Karimi M T, Ansari M, Faghih Jouibari M. Evaluating the Efficiency of Milwaukee Brace on Scoliosis Deformity: A Systematic Review of Literature. Iranian Rehabilitation Journal 2025; 23 (3) :247-256
URL: http://irj.uswr.ac.ir/article-1-2086-en.html
URL: http://irj.uswr.ac.ir/article-1-2086-en.html
1- Orthopaedic and Rehabilitation Sciences Research Center, Shiraz University of Medical Sciences, Shiraz, Iran.
2- Sports Medicine Research Center, Neuroscience Institute, Tehran University of Medical Sciences, Tehran, Iran.
3- Department of Neurosurgery, Shariati Hospital, Tehran University of Medical Sciences, Tehran, Iran.
2- Sports Medicine Research Center, Neuroscience Institute, Tehran University of Medical Sciences, Tehran, Iran.
3- Department of Neurosurgery, Shariati Hospital, Tehran University of Medical Sciences, Tehran, Iran.
Full-Text [PDF 518 kb]
(881 Downloads)
| Abstract (HTML) (2262 Views)
Full-Text: (321 Views)
Introduction
Scoliosis is defined as a three-dimensional deformity of the spine, characterized by the misalignment of the spine in the sagittal and coronal planes, associated with abnormal rotation of the spine [1]. It can be divided into two types: Structural and non-structural. The incidence of this deformity ranges from 2% to 13.6% in various countries [1, 2]. Although the primary cause of scoliosis is not well understood, several factors, such as genetics, growth, hormonal dysfunction, changes in bone mineral density, abnormalities in tissue, central nervous system abnormalities, and biomechanical factors, contribute to the incidence of this disease [3].
The treatment methods selected for scoliosis patients vary and depend on several factors, such as age, severity of the curvature, rate of progression, and location of the curve [3, 4]. Most clinicians attempt to decrease the incidence of curve progression using conservative approaches. One of the most commonly selected conservative approaches for individuals with scoliosis is the use of braces. Various types of braces have been designed for individuals with scoliosis, including the Milwaukee brace (MB), Boston brace, Cheneau braces (Rigo Cheneau, Cheneau light, Gensingen, Cheneau Toulouse Munster), Triac, C-brace, scoliosis Lycra, SpineCor, Charleston bending brace, long lever scoliosis brace, Providence, Sferzesco, Lapadula, Sibilla, Dynamic derotational brace, progressive action short brace, Spinealite soft brace, asymmetrical rigid torsion (ART) brace, Lyon, and Wilmington braces [5-10].
MB is the first modern brace designed for individuals with scoliosis. Blount and Schmidt developed the brace for post-operative treatment of post-polio scoliosis [11, 12]. The design of this brace is based on the concept that lumbar lordosis should be flattened to correct scoliosis deformity (scoliosis may be due to hypokyphosis). Scoliosis correction may be achieved through the enhancement of two active and passive mechanisms. Based on a passive mechanism, scoliosis correction can be achieved using pads or a brace’s traction [13]. However, due to the pressure applied to the body through the pads, the participants attempted to move their bodies away from the pads by actively contracting their trunk musculature.
The primary objective of using an orthosis for individuals with scoliosis is to control curve progression and subsequently decrease the scoliotic curve [3, 4]. An early report on MB efficiency supported the potential of this brace to alter the natural history of adolescent idiopathic scoliosis (AIS) and prevent curve progression. However, following up with patients over a long period showed that although some corrections could be achieved at the end of bracing, the curve tended to continually increase toward the pretreatment angle [13].
Two designs are available for MB. In the first design of the brace, correction of the curve was achieved through the use of external transverse loads applied on the apex of the curve by the use of transverse pads and vertical traction through external pressure on the mandible and the iliac crest [12-15]. Due to the side effects of traction (including alternation in facial development and vertical growth in the anterior portion of the face) in the new design, correction is achieved through the use of only transverse loads [14, 16].
The amount of MB efficiency required to control the progression of the scoliosis curve and alter the natural history of scoliosis has not been well determined. Moreover, it is crucial to determine which design of MB is more effective and has fewer side effects. The output of this review may be used to improve the design of braces for individuals with scoliosis. Therefore, this study aimed to determine the efficiency of MB in managing curve progression and curve control in patients with scoliosis based on the available literature.
Materials and Methods
This study was conducted using several databases, including Google Scholar, ISI Web of Science, PubMed, Ebsco, Embase, and Scopus, over a period between 1960 and 2024. Some keywords, such as Milwaukee orthosis and Milwaukee brace, were used in combination with scoliosis. The first selection of papers was based on the keywords above. The second selection of papers was based on their titles and abstracts, as well as whether the papers were published in English. The methodology of papers was evaluated to include the population, intervention, comparison, and outcomes. Moreover, the quality of the papers was evaluated using the Downs and Black tool. The validity and reliability of this tool were evaluated in various studies [17].
Results
Based on the keywords above, 35 studies were identified. After screening based on titles and abstracts, 21 papers were selected for the final analysis. The available studies were categorized based on the following criteria.
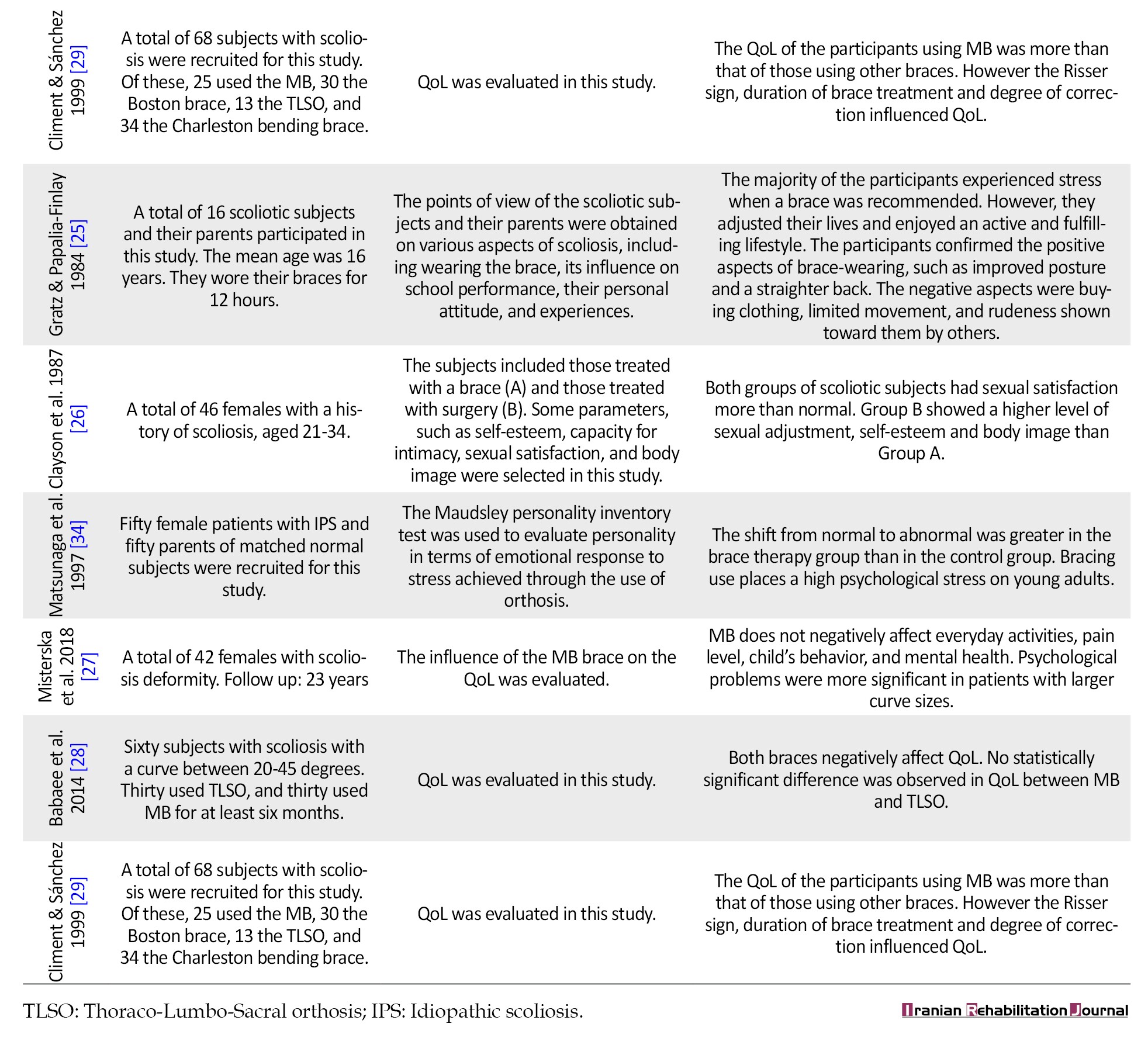
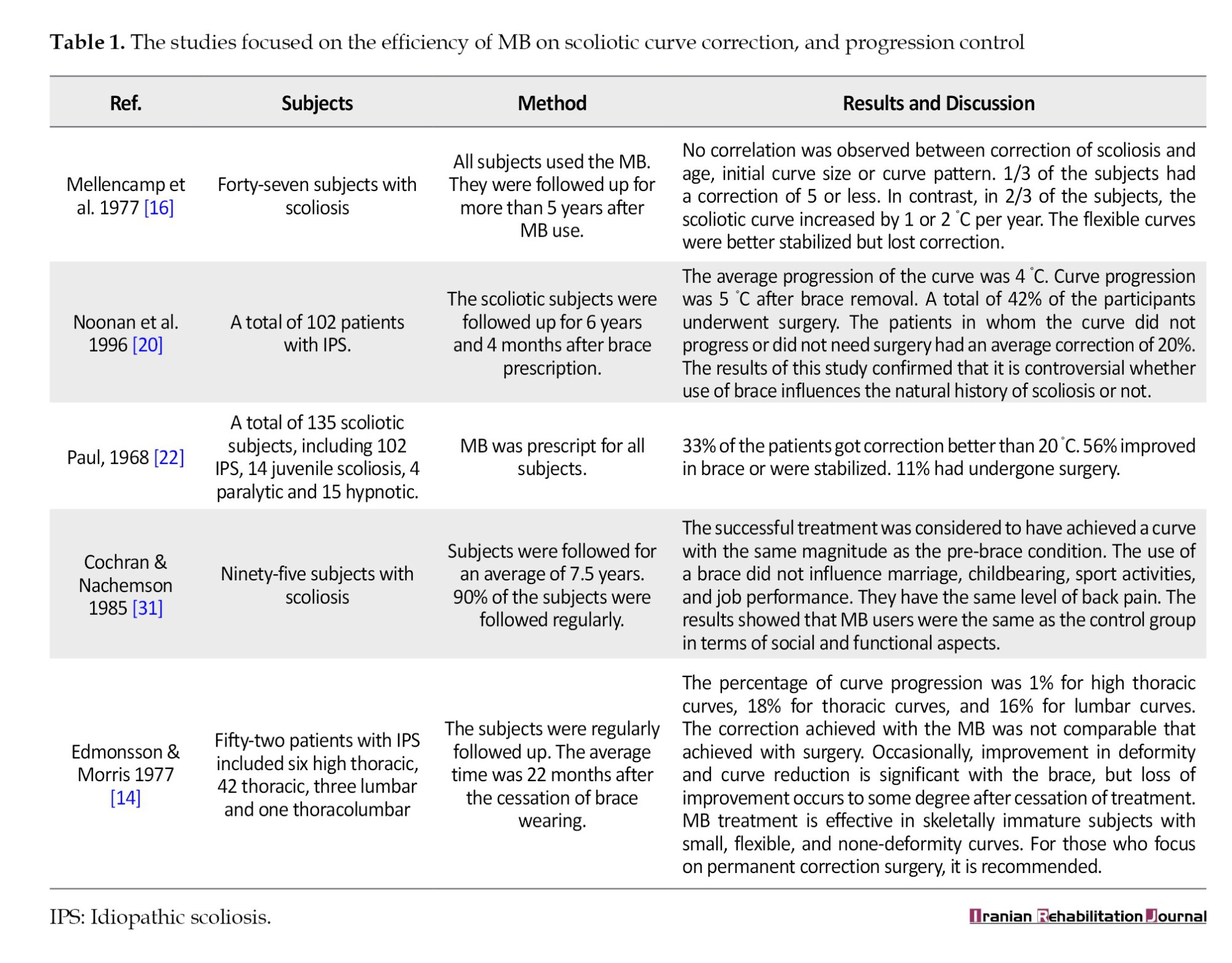
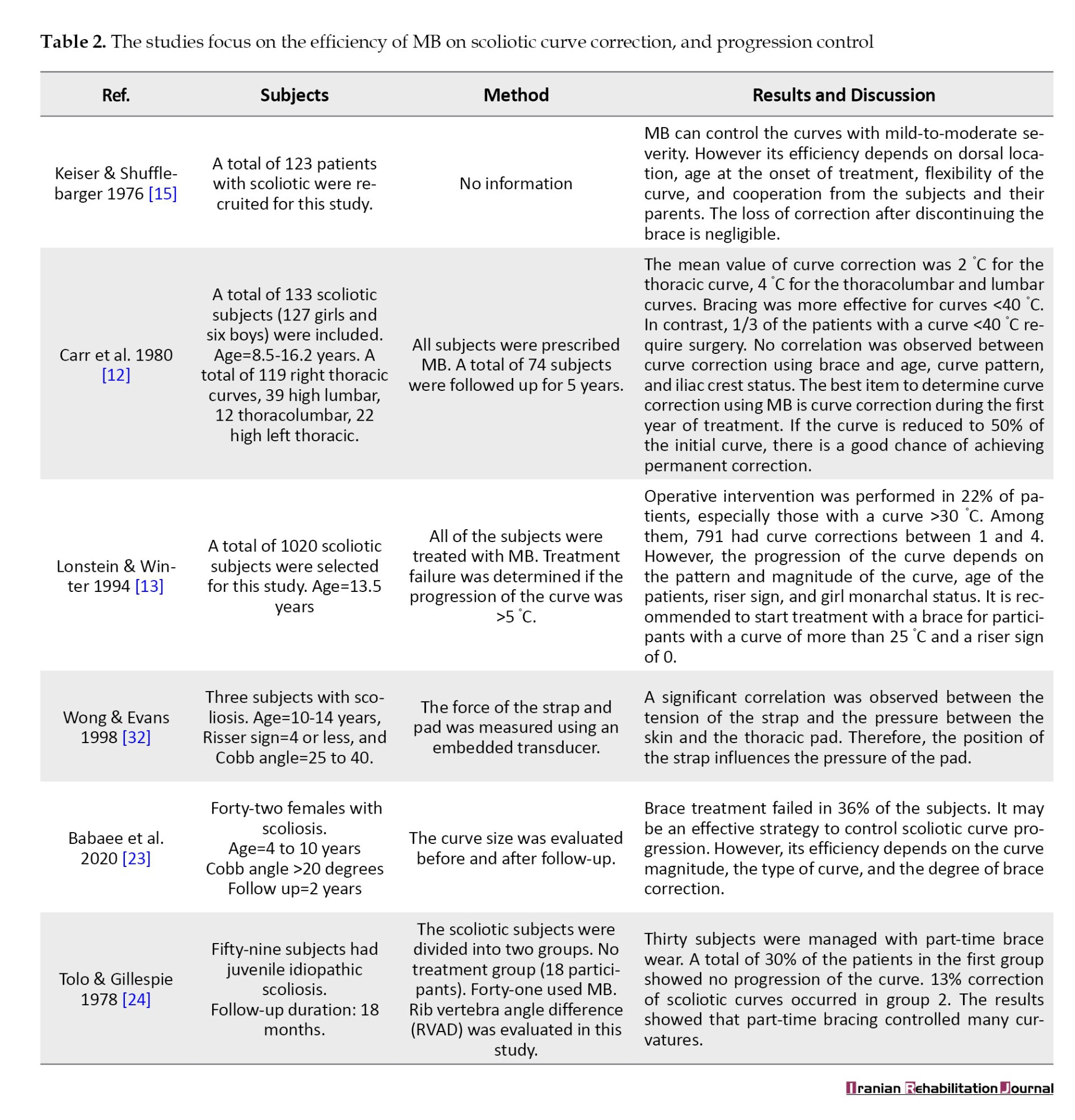
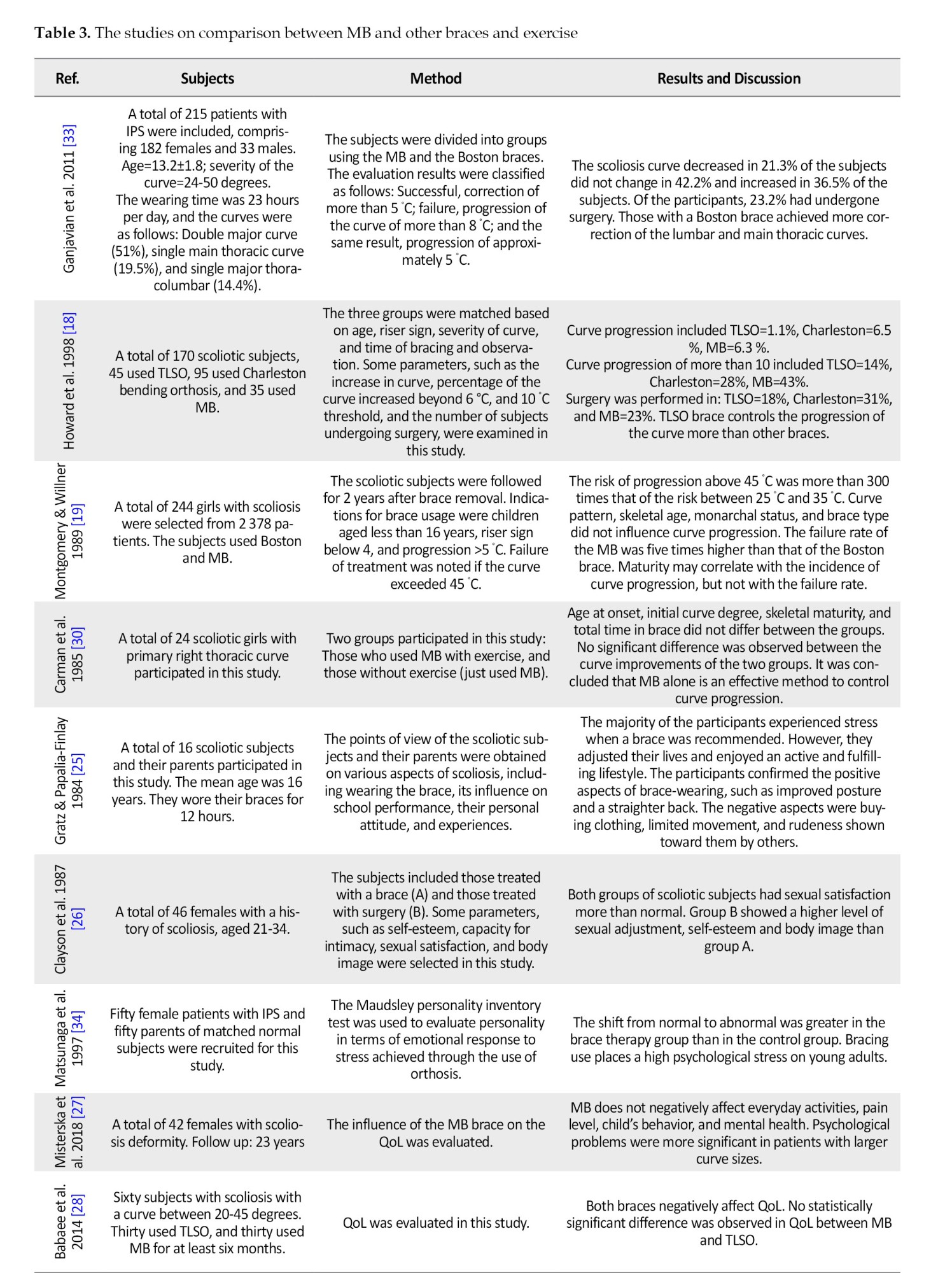
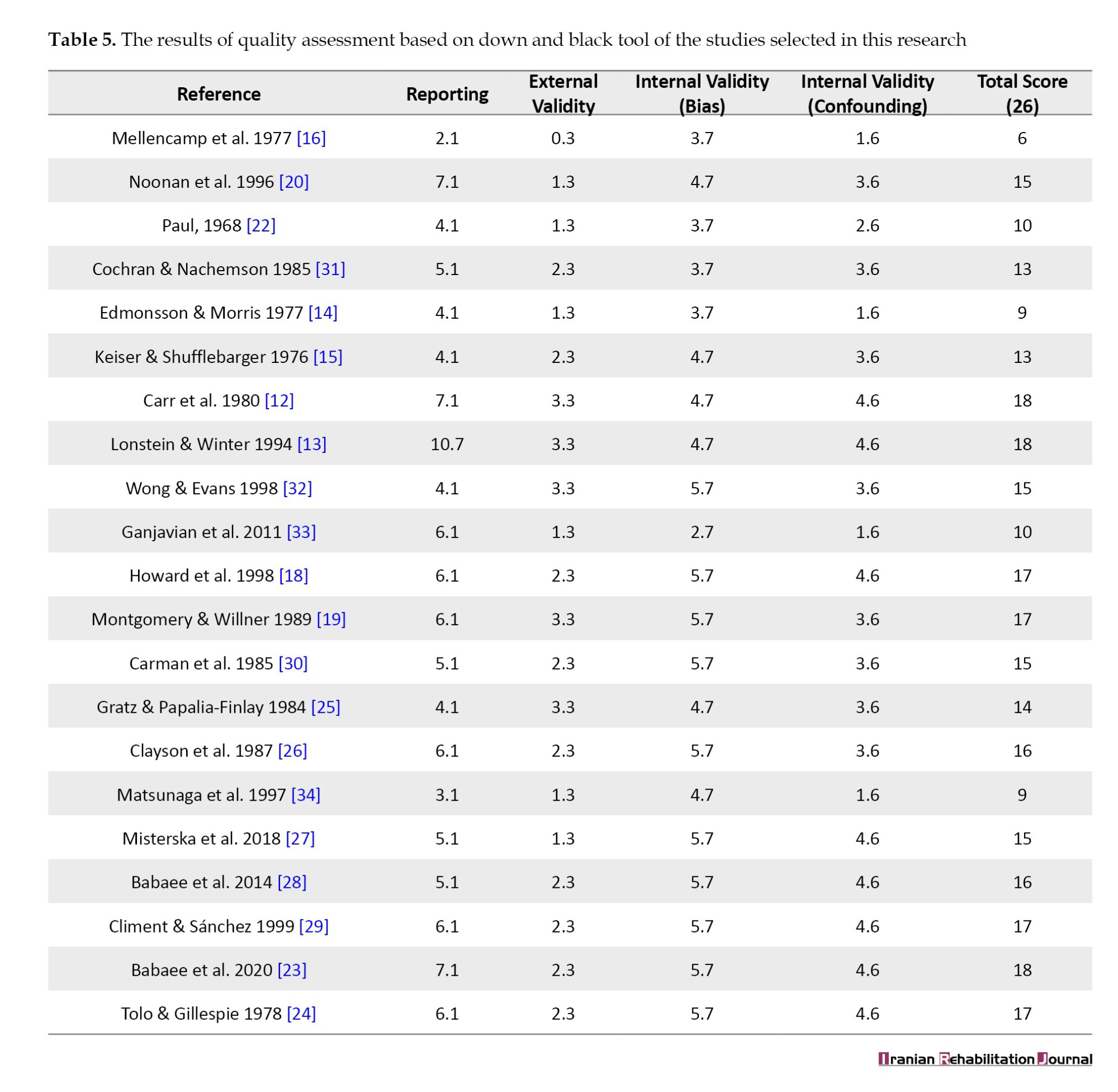
1) Papers on the efficiency of MB [10]; 2) Psychological and quality of life (QoL) of the subjects treated with MB [5]; 3) Comparison between the efficiency of Milwaukee and other orthoses [2]; 4) Combination of exercise and brace [1]. The quality of the studies varied from 6 to 18. Tables 1, 2, 3, 4 and 5 summarize the methods used in these studies and the results of the quality assessment.


Discussion
Various conservative treatment approaches have been used for patients with scoliosis deformity. The use of various orthotic designs has been recommended for this group of patients, with the MB being one of the most commonly used braces. This review aimed to collect and evaluate the evidence regarding the efficiency of MB on scoliosis. The available papers on MB can be further divided into those on the efficiency of the brace, those on comparisons with other braces, those on psychological aspects and QoL, review articles on MB, and those on the combination of MB with other therapeutic methods.
The first questions posted here are: Is MB effective in controlling curve progression and reducing curves, and which parameters influence the efficiency of MB? There were 11 studies on the efficiency of MB in scoliosis curves. The quality of most of the studies was acceptable based on the Down and Black tool. Regarding the efficiency of MB on scoliosis curves, some points should be acknowledged.
How can the efficiency of an orthosis be determined? The efficiency of MB is determined based on the progression of the curve or the number of patients who underwent surgery [12-14, 18, 19]. Moreover, treatment failure was determined if the progression of the curve exceeded 5 degrees. Edmonsson and Morris showed that braces are effective in skeletally immature patients with a small, flexible curve [14]. Moreover, Keiser and Shufflebarger confirmed that MB is effective in controlling and correcting mild to moderate idiopathic scoliosis [15]. The loss of correction after discontinuing the brace is negligible. In contrast, Lonstein and Winter showed that 22% of the subjects underwent operative intervention, especially for those with a curve greater than 30 °C [13]. Noonan et al. have shown that the use of MB is controversial regarding its influence on the natural history of scoliosis [20]. It should be emphasized that there are two designs for MB. In the first design, a combination of transverse load and vertical traction was used [11, 12]. However, due to its effect on the tempomandibular joint, only transverse loads were applied in the new design [21]. Therefore, the high efficiency of MB, as mentioned by some researchers, may be related to the first design approach [14, 16, 22]. However, a new MB design was used in other studies [20]. In a study conducted by Babaee et al., 75 individuals with scoliosis were followed for 2 years. A total of 36% of participants underwent surgery. MB was used to control the curve progression in the other subjects. The results of this study showed that MB is effective in controlling the progression of scoliotic curves. However, its efficiency depends on the curve magnitude, the type of the curve, and the degree of brace correction [23]. Tolo et al. also showed that part-time bracing (MB) can control scoliotic curve progression, depending on the severity of the curve [24]. Therefore, MB could control curve progression in scoliotic subjects depending on the type of design and may also influence the natural history of scoliosis.
Based on the available literature, the efficiency of MB on scoliosis curves depends on the location of the curve, the age of the subjects, the flexibility of the curve, and the cooperation of the subjects and their parents. Lonstein showed that progression of scoliotic curve depends on the pattern and magnitude of the curve, age of the patients, riser sign, and in girls’ monocular status [13]. Babaee et al. also showed that MB is an effective strategy to control scoliotic curve progression; however, its efficiency depends on the curve magnitude, curve type, and degree of brace correction [23]. In contrast, Carr et al. showed no correlation between age, curve pattern, and iliac crest status [12]. Montgomery and Willner also obtained the same finding, namely that there should be no correlation between correction and age, initial curve size, or curve pattern [19]. However, it should be noted that a more flexible curve can be better stabilized but loses correction [15]. Based on the studies mentioned above, the efficiency of MB may depend on factors such as, age, location, curve flexibility, and maturation status of the subjects. Therefore, MB could influence curve progression in scoliotic subjects. Although the efficiency of MB depends on the age of the subjects, the type of the curve, the riser sign, and the magnitude of the curve, the difference between the outputs of treatment with MB also depends on its design.
Based on the above-mentioned studies, MB could influence curve progression. The other crucial question is: What are the effects of MB on psychological health and QoL? The quality ratings of the six studies on this topic ranged from 9 to 16. In a study conducted by Gratz and Papalia-Finlay, 16 MB users and their parents were interviewed regarding their braces and various aspects of scoliosis, as well as the influence of the braces on school performance. They confirmed that although they were initially depressed with their brace, they could adjust their performance during daily activities [26]. In another study conducted by Clayson et al., the body image, self-esteem, and sexual satisfaction of two groups of scoliotic subjects treated with MB and surgery were compared with those of normal subjects [26]. The results showed that both groups of subjects had a higher level of sexual satisfaction than normal; however, those who underwent surgery showed a higher level of sexual adjustment and self-esteem [26]. Gratz also showed that although the participants had received a shock after wearing the brace, they confirmed that wearing the brace improved their posture and straightened their back [25]. The perception of trunk disfiguration, self-image, mental health, pain level, and activities of daily living were evaluated in 42 women after 23 years of MB use. The results of this study showed that scoliosis treated conservatively did not have a negative influence on everyday activities, pain levels, the child’s behavior and mental health [27]. In a study conducted by Babaee et al., a group of individuals treated with MB and Thoraco-Lumbo-sacral orthosis (TLSO) were followed for at least 6 months. They showed that although both braces negatively affect QoL, no significant difference was observed between the QoL of scoliotic individuals treated with MB and TLSO [28]. Clinment et al. studied the effects of MB, Boston brace, TLSO, and Charleston bending brace on the QoL of scoliotic patients. The results of this study showed that QoL score of the subjects was higher with MB. However, the Risser sign, duration of brace use, and degree of correction influence QoL [29].
Therefore, based on the aforementioned studies, MB does not have a significant effect on the psychological health of scoliotic subjects and their parents. Furthermore, it did not influence their daily activities or self-image.
The other question posted here is whether there is any difference between the treatment outputs achieved with MB compared to those with other braces. The quality ratings of the three studies on this topic ranged from 10 to 17. The quality of these studies was high due to the big large number of participants. In a study conducted by Howard on 170 scoliotic subjects, 45 used a TLSO, 95 used a Charleston bending orthosis, and 35 used an MB [18]. The treatment output was scored based on the progression of the curve and the number of participants who underwent surgery. The results confirmed that MB had a five-times greater risk of failure than the Boston brace [18]. The risk of failure of brace treatment for a curve more than 45 °C was 300 times greater than that for an initial curve between 25 °C and 35 °C. Moreover, they confirmed that the vital parameter to predict the failure of the brace is the initial curve magnitude [18]. Carman et al. checked the combination of exercise and use of MB on the scoliosis curve. They confirmed that the use of MB is enough to decrease the progression of the scoliosis curve [30]. From the above-mentioned studies and due to quality of the studies, it can be concluded that Boston brace which is a total contact brace may be more effective for scoliotic subjects. However, it should be noted that it can only be used for curves below T8. The primary feature of the Boston brace design is its total contact structure, which applies a transverse force and traction along the curve. Another point that should be emphasized is that the new MB design was used for the participants in these studies.
However, there are some limitations to the available studies. The main limitation associated with the available studies was limited information regarding the type of MB used. Moreover, in most studies, the efficiency of the brace was determined after a follow-up period. No information was available regarding in-brace correction. Finally, the follow-up duration varied significantly among the studies.
Based on the above-mentioned studies, MB could decrease scoliosis curve progression. The efficiency of the MB depends on the type of curve, location of the curve, flexibility, age of the subjects, and riser sign. The effectiveness of other orthoses seems to be better than MB, possibly due to their designs, which allow for total contact and the simultaneous application of transverse and traction forces. It should be emphasized that the efficiency of MB differs between the new and old designs. Although the efficiency of the old design is better than the new design, it has some side effects. Therefore, it is recommended that, due to the adjustability of the MB and its wide usage for all scoliotic curves, a new type of this brace be developed to use both transverse and traction load configurations.
Conclusion
Available studies on MB were compiled using a systematic approach. The results of the quality assessment showed that most studies had a high degree of quality due to the large number of subjects, and long follow-up duration. The results of these studies showed that MB decreased the progression of scoliotic curve. The efficiency of the older design of the MB and other TLSO orthoses is greater than that of the new design of the MB. It is recommended that, due to the adjustability of MB and its advantages, a new type of MB be developed to incorporate both transverse and traction to straighten the scoliotic curve.
Ethical Considerations
Compliance with ethical guidelines
There were no ethical considerations to be considered in this research.
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
Investigation: Majid Ansari; Quality assessment: Majid Ansari and Morteza Faghih Jouibari; Writing the original draft: Morteza Faghih Jouibari; Supervision, review and editing: Mohammad Taghi Karimi.
Conflict of interest
The authors declared no conflict of interest.
References
Scoliosis is defined as a three-dimensional deformity of the spine, characterized by the misalignment of the spine in the sagittal and coronal planes, associated with abnormal rotation of the spine [1]. It can be divided into two types: Structural and non-structural. The incidence of this deformity ranges from 2% to 13.6% in various countries [1, 2]. Although the primary cause of scoliosis is not well understood, several factors, such as genetics, growth, hormonal dysfunction, changes in bone mineral density, abnormalities in tissue, central nervous system abnormalities, and biomechanical factors, contribute to the incidence of this disease [3].
The treatment methods selected for scoliosis patients vary and depend on several factors, such as age, severity of the curvature, rate of progression, and location of the curve [3, 4]. Most clinicians attempt to decrease the incidence of curve progression using conservative approaches. One of the most commonly selected conservative approaches for individuals with scoliosis is the use of braces. Various types of braces have been designed for individuals with scoliosis, including the Milwaukee brace (MB), Boston brace, Cheneau braces (Rigo Cheneau, Cheneau light, Gensingen, Cheneau Toulouse Munster), Triac, C-brace, scoliosis Lycra, SpineCor, Charleston bending brace, long lever scoliosis brace, Providence, Sferzesco, Lapadula, Sibilla, Dynamic derotational brace, progressive action short brace, Spinealite soft brace, asymmetrical rigid torsion (ART) brace, Lyon, and Wilmington braces [5-10].
MB is the first modern brace designed for individuals with scoliosis. Blount and Schmidt developed the brace for post-operative treatment of post-polio scoliosis [11, 12]. The design of this brace is based on the concept that lumbar lordosis should be flattened to correct scoliosis deformity (scoliosis may be due to hypokyphosis). Scoliosis correction may be achieved through the enhancement of two active and passive mechanisms. Based on a passive mechanism, scoliosis correction can be achieved using pads or a brace’s traction [13]. However, due to the pressure applied to the body through the pads, the participants attempted to move their bodies away from the pads by actively contracting their trunk musculature.
The primary objective of using an orthosis for individuals with scoliosis is to control curve progression and subsequently decrease the scoliotic curve [3, 4]. An early report on MB efficiency supported the potential of this brace to alter the natural history of adolescent idiopathic scoliosis (AIS) and prevent curve progression. However, following up with patients over a long period showed that although some corrections could be achieved at the end of bracing, the curve tended to continually increase toward the pretreatment angle [13].
Two designs are available for MB. In the first design of the brace, correction of the curve was achieved through the use of external transverse loads applied on the apex of the curve by the use of transverse pads and vertical traction through external pressure on the mandible and the iliac crest [12-15]. Due to the side effects of traction (including alternation in facial development and vertical growth in the anterior portion of the face) in the new design, correction is achieved through the use of only transverse loads [14, 16].
The amount of MB efficiency required to control the progression of the scoliosis curve and alter the natural history of scoliosis has not been well determined. Moreover, it is crucial to determine which design of MB is more effective and has fewer side effects. The output of this review may be used to improve the design of braces for individuals with scoliosis. Therefore, this study aimed to determine the efficiency of MB in managing curve progression and curve control in patients with scoliosis based on the available literature.
Materials and Methods
This study was conducted using several databases, including Google Scholar, ISI Web of Science, PubMed, Ebsco, Embase, and Scopus, over a period between 1960 and 2024. Some keywords, such as Milwaukee orthosis and Milwaukee brace, were used in combination with scoliosis. The first selection of papers was based on the keywords above. The second selection of papers was based on their titles and abstracts, as well as whether the papers were published in English. The methodology of papers was evaluated to include the population, intervention, comparison, and outcomes. Moreover, the quality of the papers was evaluated using the Downs and Black tool. The validity and reliability of this tool were evaluated in various studies [17].
Results
Based on the keywords above, 35 studies were identified. After screening based on titles and abstracts, 21 papers were selected for the final analysis. The available studies were categorized based on the following criteria.
1) Papers on the efficiency of MB [10]; 2) Psychological and quality of life (QoL) of the subjects treated with MB [5]; 3) Comparison between the efficiency of Milwaukee and other orthoses [2]; 4) Combination of exercise and brace [1]. The quality of the studies varied from 6 to 18. Tables 1, 2, 3, 4 and 5 summarize the methods used in these studies and the results of the quality assessment.






Discussion
Various conservative treatment approaches have been used for patients with scoliosis deformity. The use of various orthotic designs has been recommended for this group of patients, with the MB being one of the most commonly used braces. This review aimed to collect and evaluate the evidence regarding the efficiency of MB on scoliosis. The available papers on MB can be further divided into those on the efficiency of the brace, those on comparisons with other braces, those on psychological aspects and QoL, review articles on MB, and those on the combination of MB with other therapeutic methods.
The first questions posted here are: Is MB effective in controlling curve progression and reducing curves, and which parameters influence the efficiency of MB? There were 11 studies on the efficiency of MB in scoliosis curves. The quality of most of the studies was acceptable based on the Down and Black tool. Regarding the efficiency of MB on scoliosis curves, some points should be acknowledged.
How can the efficiency of an orthosis be determined? The efficiency of MB is determined based on the progression of the curve or the number of patients who underwent surgery [12-14, 18, 19]. Moreover, treatment failure was determined if the progression of the curve exceeded 5 degrees. Edmonsson and Morris showed that braces are effective in skeletally immature patients with a small, flexible curve [14]. Moreover, Keiser and Shufflebarger confirmed that MB is effective in controlling and correcting mild to moderate idiopathic scoliosis [15]. The loss of correction after discontinuing the brace is negligible. In contrast, Lonstein and Winter showed that 22% of the subjects underwent operative intervention, especially for those with a curve greater than 30 °C [13]. Noonan et al. have shown that the use of MB is controversial regarding its influence on the natural history of scoliosis [20]. It should be emphasized that there are two designs for MB. In the first design, a combination of transverse load and vertical traction was used [11, 12]. However, due to its effect on the tempomandibular joint, only transverse loads were applied in the new design [21]. Therefore, the high efficiency of MB, as mentioned by some researchers, may be related to the first design approach [14, 16, 22]. However, a new MB design was used in other studies [20]. In a study conducted by Babaee et al., 75 individuals with scoliosis were followed for 2 years. A total of 36% of participants underwent surgery. MB was used to control the curve progression in the other subjects. The results of this study showed that MB is effective in controlling the progression of scoliotic curves. However, its efficiency depends on the curve magnitude, the type of the curve, and the degree of brace correction [23]. Tolo et al. also showed that part-time bracing (MB) can control scoliotic curve progression, depending on the severity of the curve [24]. Therefore, MB could control curve progression in scoliotic subjects depending on the type of design and may also influence the natural history of scoliosis.
Based on the available literature, the efficiency of MB on scoliosis curves depends on the location of the curve, the age of the subjects, the flexibility of the curve, and the cooperation of the subjects and their parents. Lonstein showed that progression of scoliotic curve depends on the pattern and magnitude of the curve, age of the patients, riser sign, and in girls’ monocular status [13]. Babaee et al. also showed that MB is an effective strategy to control scoliotic curve progression; however, its efficiency depends on the curve magnitude, curve type, and degree of brace correction [23]. In contrast, Carr et al. showed no correlation between age, curve pattern, and iliac crest status [12]. Montgomery and Willner also obtained the same finding, namely that there should be no correlation between correction and age, initial curve size, or curve pattern [19]. However, it should be noted that a more flexible curve can be better stabilized but loses correction [15]. Based on the studies mentioned above, the efficiency of MB may depend on factors such as, age, location, curve flexibility, and maturation status of the subjects. Therefore, MB could influence curve progression in scoliotic subjects. Although the efficiency of MB depends on the age of the subjects, the type of the curve, the riser sign, and the magnitude of the curve, the difference between the outputs of treatment with MB also depends on its design.
Based on the above-mentioned studies, MB could influence curve progression. The other crucial question is: What are the effects of MB on psychological health and QoL? The quality ratings of the six studies on this topic ranged from 9 to 16. In a study conducted by Gratz and Papalia-Finlay, 16 MB users and their parents were interviewed regarding their braces and various aspects of scoliosis, as well as the influence of the braces on school performance. They confirmed that although they were initially depressed with their brace, they could adjust their performance during daily activities [26]. In another study conducted by Clayson et al., the body image, self-esteem, and sexual satisfaction of two groups of scoliotic subjects treated with MB and surgery were compared with those of normal subjects [26]. The results showed that both groups of subjects had a higher level of sexual satisfaction than normal; however, those who underwent surgery showed a higher level of sexual adjustment and self-esteem [26]. Gratz also showed that although the participants had received a shock after wearing the brace, they confirmed that wearing the brace improved their posture and straightened their back [25]. The perception of trunk disfiguration, self-image, mental health, pain level, and activities of daily living were evaluated in 42 women after 23 years of MB use. The results of this study showed that scoliosis treated conservatively did not have a negative influence on everyday activities, pain levels, the child’s behavior and mental health [27]. In a study conducted by Babaee et al., a group of individuals treated with MB and Thoraco-Lumbo-sacral orthosis (TLSO) were followed for at least 6 months. They showed that although both braces negatively affect QoL, no significant difference was observed between the QoL of scoliotic individuals treated with MB and TLSO [28]. Clinment et al. studied the effects of MB, Boston brace, TLSO, and Charleston bending brace on the QoL of scoliotic patients. The results of this study showed that QoL score of the subjects was higher with MB. However, the Risser sign, duration of brace use, and degree of correction influence QoL [29].
Therefore, based on the aforementioned studies, MB does not have a significant effect on the psychological health of scoliotic subjects and their parents. Furthermore, it did not influence their daily activities or self-image.
The other question posted here is whether there is any difference between the treatment outputs achieved with MB compared to those with other braces. The quality ratings of the three studies on this topic ranged from 10 to 17. The quality of these studies was high due to the big large number of participants. In a study conducted by Howard on 170 scoliotic subjects, 45 used a TLSO, 95 used a Charleston bending orthosis, and 35 used an MB [18]. The treatment output was scored based on the progression of the curve and the number of participants who underwent surgery. The results confirmed that MB had a five-times greater risk of failure than the Boston brace [18]. The risk of failure of brace treatment for a curve more than 45 °C was 300 times greater than that for an initial curve between 25 °C and 35 °C. Moreover, they confirmed that the vital parameter to predict the failure of the brace is the initial curve magnitude [18]. Carman et al. checked the combination of exercise and use of MB on the scoliosis curve. They confirmed that the use of MB is enough to decrease the progression of the scoliosis curve [30]. From the above-mentioned studies and due to quality of the studies, it can be concluded that Boston brace which is a total contact brace may be more effective for scoliotic subjects. However, it should be noted that it can only be used for curves below T8. The primary feature of the Boston brace design is its total contact structure, which applies a transverse force and traction along the curve. Another point that should be emphasized is that the new MB design was used for the participants in these studies.
However, there are some limitations to the available studies. The main limitation associated with the available studies was limited information regarding the type of MB used. Moreover, in most studies, the efficiency of the brace was determined after a follow-up period. No information was available regarding in-brace correction. Finally, the follow-up duration varied significantly among the studies.
Based on the above-mentioned studies, MB could decrease scoliosis curve progression. The efficiency of the MB depends on the type of curve, location of the curve, flexibility, age of the subjects, and riser sign. The effectiveness of other orthoses seems to be better than MB, possibly due to their designs, which allow for total contact and the simultaneous application of transverse and traction forces. It should be emphasized that the efficiency of MB differs between the new and old designs. Although the efficiency of the old design is better than the new design, it has some side effects. Therefore, it is recommended that, due to the adjustability of the MB and its wide usage for all scoliotic curves, a new type of this brace be developed to use both transverse and traction load configurations.
Conclusion
Available studies on MB were compiled using a systematic approach. The results of the quality assessment showed that most studies had a high degree of quality due to the large number of subjects, and long follow-up duration. The results of these studies showed that MB decreased the progression of scoliotic curve. The efficiency of the older design of the MB and other TLSO orthoses is greater than that of the new design of the MB. It is recommended that, due to the adjustability of MB and its advantages, a new type of MB be developed to incorporate both transverse and traction to straighten the scoliotic curve.
Ethical Considerations
Compliance with ethical guidelines
There were no ethical considerations to be considered in this research.
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
Investigation: Majid Ansari; Quality assessment: Majid Ansari and Morteza Faghih Jouibari; Writing the original draft: Morteza Faghih Jouibari; Supervision, review and editing: Mohammad Taghi Karimi.
Conflict of interest
The authors declared no conflict of interest.
References
- Rogala EJ, Drummond DS, Gurr J. Scoliosis: Incidence and natural history. A prospective epidemiological study.The Journal of Bone and Joint Surgery. American Volume. 1978; 60(2):173-6. [DOI:10.2106/00004623-197860020-00005] [PMID]
- Ma X, Zhao B, Lin QK. [Investigation on scoliosis incidence among 24,130 school children (Chinese)]. Zhonghua Liuxingbingxue Zazhi. 1995; 16(2):109-10. [PMID]
- Goldberg CJ, Moore DP, Fogarty EE, Dowling FE. Scoliosis: A review. Pediatric surgery International. 2008; 24(2):129-44. [DOI:10.1007/s00383-007-2016-5] [PMID]
- Janicki JA, Alman B. Scoliosis: Review of diagnosis and treatment. Paediatrics & Child Health. 2007; 12(9):771-6. [DOI:10.1093/pch/12.9.771] [PMID]
- Grivas TB, Kaspiris A. European braces widely used for conservative scoliosis treatment. Studies in Health Technology and Informatics. 2010; 158:157-66. [PMID]
- Zaborowska-Sapeta K, Kowalski IM, Kotwicki T, Protasiewicz-Fałdowska H, Kiebzak W. Effectiveness of Chêneau brace treatment for idiopathic scoliosis: Prospective study in 79 patients followed to skeletal maturity. Scoliosis. 2011; 6(1):2. [DOI:10.1186/1748-7161-6-2] [PMID]
- Zeh A, Planert M, Klima S, Hein W, Wohlrab D. The flexible Triac-Brace for conservative treatment of idiopathic scoliosis. An alternative treatment option? Acta Orthopaedica Belgica. 2008; 74(4):512-21. [PMID]
- Weiss HR, Werkmann M. "Brace Technology" Thematic Series - The ScoliOlogiC® Chêneau light™ brace in the treatment of scoliosis. Scoliosis. 2010; 5:19. [DOI:10.1186/1748-7161-5-19] [PMID]
- Weiss HR. "Brace technology" thematic series - the Gensingen brace™ in the treatment of scoliosis. Scoliosis. 2010; 5:22. [DOI:10.1186/1748-7161-5-22] [PMID]
- van Loon PJ, Roukens M, Kuit JDj, Thunnissen FB. A new brace treatment similar for adolescent scoliosis and kyphosis based on restoration of thoracolumbar lordosis. Radiological and subjective clinical results after at least one year of treatment. Scoliosis. 2012; 7(1):19. [DOI:10.1186/1748-7161-7-19] [PMID]
- Blount WP, Schmidt AC, Keever ED, Leonard ET. The Milwaukee brace in the operative treatment of scoliosis. The Journal of Bone and Joint Surgery. American Volume. 1958; 40-A(3):511-25. [DOI:10.2106/00004623-195840030-00003] [PMID]
- Carr WA, Moe JH, Winter RB, Lonstein JE. Treatment of idiopathic scoliosis in the Milwaukee brace. The Journal of Bone and Joint Surgery. American Volume. 1980; 62(4):599-612. [DOI:10.2106/00004623-198062040-00015] [PMID]
- Lonstein JE, Winter RB. The Milwaukee brace for the treatment of adolescent idiopathic scoliosis. A review of one thousand and twenty patients. The Journal of Bone and Joint Surgery. American Volume. 1994; 76(8):1207-21. [DOI:10.2106/00004623-199408000-00011] [PMID]
- Edmonsson AS, Morris JT. Follow-up study of Milwaukee brace treatment in patients with idiopathic scoliosis. Clinical Orthopaedics and Related Research. 1977; (126):58-61. [DOI:10.1097/00003086-197707000-00008] [PMID]
- Keiser RP, Shufflebarger HL. The Milwaukee brace in idiopathic scoliosis: Evaluation of 123 completed cases. Clinical Orthopaedics and Related Research. 1976; (118):19-24. [DOI:10.1097/00003086-197607000-00005]
- Mellencamp DD, Blount WP, Anderson AJ. Milwaukee brace treatment of idiopathic scoliosis: Late results. Clinical Orthopaedics and Related Research. 1977; (126):47-57. [DOI:10.1097/00003086-197707000-00007] [PMID]
- Downs SH, Black N. The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. Journal of Epidemiology and Community Health. 1998; 52(6):377-84. [DOI:10.1136/jech.52.6.377]
- Howard A, Wright JG, Hedden D. A comparative study of TLSO, Charleston, and Milwaukee braces for idiopathic scoliosis. Spine (Phila Pa 1976). 1998; 23(22):2404-11. [DOI:10.1097/00007632-199811150-00009] [PMID]
- Montgomery F, Willner S. Prognosis of brace-treated scoliosis: Comparison of the Boston and Milwaukee methods in 244 girls. Acta Orthopaedica Scandinavica. 1989; 60(4):383-5. [DOI:10.3109/17453678909149302]
- Noonan KJ, Weinstein SL, Jacobson WC, Dolan LA. Use of the Milwaukee brace for progressive idiopathic scoliosis. The Journal of Bone and Joint Surgery. American Volume. 1996; 78(4):557-67. [DOI:10.2106/00004623-199604000-00009] [PMID]
- Saccucci M, Tettamanti L, Mummolo S, Polimeni A, Festa F, Tecco S. Scoliosis and dental occlusion: A review of the literature. Scoliosis. 2011; 6:15. [DOI:10.1186/1748-7161-6-15]
- Paul SW. Five years of nonoperative treatment of scoliosis and kyphosis: A follow-up study. Orthotics and Prosthetics. 1968; 22:28-45. [Link]
- Babaee T, Kamyab M, Ganjavian MS, Rouhani N, Jarvis J. Success rate of brace treatment for juvenile-onset idiopathic scoliosis up to skeletal maturity. International Journal of Spine Surgery. 2020; 14(5):824-31. [DOI:10.14444/7117] [PMID]
- Tolo V, Gillespie R. The characteristics of juvenile idiopathic scoliosis and results of its treatment. The Journal of Bone & Joint Surgery British Volume 1978; 60-B(2):181-8.[DOI:10.1302/0301-620X.60B2.659460]
- Gratz RR, Papalia-Finlay D. Psychosocial adaptation to wearing the Milwaukee brace for scoliosis. A pilot study of adolescent females and their mothers. Journal of Adolescent Health Care. 1984; 5(4):237-42. [DOI:10.1016/S0197-0070(84)80124-2]
- Clayson D, Luz-Alterman S, Cataletto MM, Levine DB. Long-term psychological sequelae of surgically versus nonsurgically treated scoliosis. Spine (Phila Pa 1976). 1987; 12(10):983-6. [DOI:10.1097/00007632-198712000-00007] [PMID]
- Misterska E, Głowacki J, Głowacki M, Okręt A. Long-term effects of conservative treatment of Milwaukee brace on body image and mental health of patients with idiopathic scoliosis. PLoS One. 2018; 13(2):e0193447. [DOI:10.1371/journal.pone.0193447] [PMID]
- Babaee T, Kamyab M, Ganjavian MS, Kamali M. Milwaukee brace or thoracolumbosacral orthosis? Which one affects the quality of life of adolescents with idiopathic scoliosis more? A cross-sectional study using the SRS-22 questionnaire. Current Orthopaedic Practice. 2014; 25(5):478-83. [DOI:10.1097/BCO.0000000000000138]
- Climent JM, Sánchez J. Impact of the type of brace on the quality of life of Adolescents with Spine Deformities. Spine (Phila Pa 1976). 1999; 24(18):1903-8. [DOI:10.1097/00007632-199909150-00007] [PMID]
- Carman D, Roach JW, Speck G, Wenger DR, Herring JA. Role of exercises in the Milwaukee brace treatment of scoliosis. Journal of Pediatric Orthopedics. 1985; 5(1):65-8. [DOI:10.1097/01241398-198501000-00011] [PMID]
- Cochran T, Nachemson A. Long-term anatomic and functional changes in patients with adolescent idiopathic scoliosis treated with the Milwaukee brace. Spine (Phila Pa 1976). 1985; 10(2):127-33. [DOI:10.1097/00007632-198503000-00003] [PMID]
- Wong MS, Evans JH. Biomechanical evaluation of the Milwaukee brace. Prosthetics and Orthotics International. 1998; 22(1):54-67. [DOI:10.3109/03093649809164457] [PMID]
- Ganjavian MS, Behtash H, Ameri E, Khakinahad M. Results of Milwaukee and Boston braces with or without metal marker around pads in patients with idiopathic scoliosis. Acta Medica Iranica. 2011; 49(9):598-605. [PMID]
- Matsunaga S, Sakou T, Nozoe S. Psychological effects of brace therapy on patients with idiopathic scoliosis. Journal of Orthopaedic Science. 1997; 2(6):391-5. [DOI:10.1007/BF02488926]
Article type: Reviews |
Subject:
Orthosis and Prosthesis
Received: 2023/09/28 | Accepted: 2025/04/28 | Published: 2025/09/1
Received: 2023/09/28 | Accepted: 2025/04/28 | Published: 2025/09/1
Send email to the article author








