Volume 23, Issue 3 (September 2025)
Iranian Rehabilitation Journal 2025, 23(3): 311-320 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Salam Dakhel Alwatify S, Radhi M M. Diabetes Health Literacy as a Mediator Between Diabetes Self-management and Medication Adherence Among Diabetic Patients. Iranian Rehabilitation Journal 2025; 23 (3) :311-320
URL: http://irj.uswr.ac.ir/article-1-2446-en.html
URL: http://irj.uswr.ac.ir/article-1-2446-en.html
1- Health Technologies Community, College of Health and Medical Techniques-Kufa, Al-Furat Al-Awsat Technical University, Babylon, Iraq.
2- Health Nursing Community, College of Health and Medical Techniques-Kufa, Al-Furat Al-Awsat Technical University, Babylon, Iraq.
2- Health Nursing Community, College of Health and Medical Techniques-Kufa, Al-Furat Al-Awsat Technical University, Babylon, Iraq.
Full-Text [PDF 621 kb]
(568 Downloads)
| Abstract (HTML) (2053 Views)
Full-Text: (260 Views)
Introduction
Diabetes is one of the health problems affecting the entire world, affecting tens of millions of people and posing major challenges to patients and health management companies [1]. Effective diabetes management requires individuals to have sufficient health literacy, which plays a pivotal role in understanding the disease, managing symptoms, and adhering to treatment regimens [2]. Health literacy is “the ability to acquire, process, and understand basic health facts and services needed to make appropriate health choices” [3]. For patients with diabetes, health literacy extends beyond general knowledge to include unique abilities in self-management and adherence to treatment, which are crucial for maintaining optimal glycemic control [4, 5].
Research has demonstrated that diabetes self-management behaviors, including blood sugar monitoring, diet regulation, and physical activity, are directly influenced by patients’ health literacy levels [6, 7]. Poor health literacy is associated with inadequate understanding of diabetes, suboptimal self-management behaviors, and poor glycemic management [8]. This highlights the need for targeted interventions that enhance health literacy, enabling patients to manage their conditions effectively [9].
Medication adherence is another crucial aspect of diabetes management that greatly intersects with health literacy [10]. Certainly, non-adherence to prescribed medications is an important limitation to achieving favorable therapeutic outcomes in chronic conditions, including diabetes [11]. Patients with low health literacy may also fail to recognize medication instructions, leading to neglected dosing or incorrect administration. This emphasizes the importance of examining how health literacy mediates the relationship between self-management and adherence [12].
Recent studies have begun to highlight the mediating role of health literacy in diabetes outcomes. Health literacy is a crucial mediator, linking diabetes self-management education to improved treatment adherence and medical outcomes. These findings suggest that improving health literacy can not only improve individual health behaviors but also promote better overall management of diabetes, reducing the long-term burden of the disease [13, 14]. Given this context, the current study investigated the mediating role of diabetes health literacy in the relationship between self-management practices and medication adherence among patients with diabetes. Building on previous studies, this study aimed to provide a deeper understanding of the complex relationships between these variables, thus contributing to the development of effective interventions to improve diabetes management outcomes.
Materials and Methods
Study design and sitting
This study used a correlational design to investigate the mediating role of diabetes health literacy in the relationship between self-management practices and medication adherence among patients with diabetes. The design was selected to examine the functional role of diabetes health literacy as a mediator between self-management and adherence behaviors, providing insights into how these variables interact. The studies were conducted at the Babylon Diabetes and Endocrinology Center, a specialized facility providing comprehensive diabetes management. This setting enabled access to various individuals managing diabetes through self-management and prescribed treatment regimens. Patients were managed during their repeated visits to the center, facilitating an efficient record chain.
Study sample
A total of 328 patients with diabetes were recruited using convenience sampling. Participants were approached during their routine visits to the center, ensuring a diverse representation of patients managing their diabetes through self-management and prescribed medication regimens. This study used a convenience sampling method to recruit 328 patients from a target population of 2 262, based on Cochran’s formula for sample size determination. This formula calculates the sample size for large populations and adjusts it for finite populations [15]. The inclusion criteria included individuals aged 18 years or older, with a diagnosis of diabetes of at least six months’ duration, who were able to provide informed consent and respond to study modules. Patients with severe complications or cognitive impairment that could interfere with their ability to participate were excluded. This ensured that the results accurately reflected the relationship between certain study variables.
Study instruments
Data were collected using two validated instruments. The diabetes self-management questionnaire (DSMQ) was used to assess patients’ self-management behaviors, covering aspects, such as glucose management, dietary management, physical activity, and healthcare utilization [16]. The medication adherence report scale (MARS) was used to assess adherence to prescribed medication regimens [17]. The diabetic health literacy scale (DHLS) was used to evaluate the diabetes-related health literacy of patients with diabetes. Both instruments are widely recognized for their reliability and validity in diabetes research.
Validity and reliability
The management fully assessed the validity and reliability of the instruments. Content validity was ensured through expert review, and reliability was tested in a pilot study involving 30 participants. The reliability of the study instruments was assessed using Cronbach’s α and the intraclass correlation coefficient (ICC). Cronbach’s α values exceeded 0.80 for all scales, indicating strong internal consistency. Additionally, ICC was calculated using a two-way mixed-effects model to assess test re-test reliability over a two-week interval. The DSMQ (ICC=0.89), MARS (ICC=0.87), and DHLS (ICC=0.91) demonstrated excellent reliability, confirming the stability and consistency of the measurements over time.
Data collection
Data collection spanned three months, during which participants were provided with questionnaires in a structured interview format. Trained research assistants administered the instruments to minimize response bias and ensure clarity in patient responses. Demographic data, such as age, sex, marital status, education level, occupation, monthly income, and duration of diabetes, were also recorded to support contextual analysis.
Data analysis
The collected data were entered into a statistical program and analyzed using descriptive and inferential statistics. Descriptive statistics, including means, frequencies, and percentages, were used to summarize demographic and clinical variables. The Kolmogorov-Smirnov test (K-S test) was used to test normality. The relationship between diabetes self-management and medication adherence was analyzed using Pearson’s correlation coefficient and simple linear regression. A significance level of P<0.05 was set for all statistical tests.
Results
In terms of statistical frequencies and percentages, Table 1 shows the socio-demographic characteristics of 328 patients who participated in this study. Their ages ranged from 21 to 68 years, with a mean age of 45.35±9.38 years. Notably, more than half of the participants were women (56.1%). The majority (80.2%) were married, (60.4%) were urban residents, (32%) were primary school graduates, (71%) were unemployed, and (38.4%) had a limited or insufficient monthly income. The duration of diabetes ranged from 1 to 28 years, with a mean duration of 9.62±6.477 years.

The results in Table 2 showed that 63.1% of the patients expressed a moderate level of diabetic self-management (34.44±5.347). Regarding treatment adherence, 58.8% of patients with diabetes exhibited good adherence (25.87±3.357). Concerning diabetic health literacy, 46.3% of patients with diabetes had a moderate level (28.12±5.861).

The results of the simple linear regression test in Table 3 indicated that health literacy can serve as a predictor of diabetic self-management (β=0.625, P=0.000) and treatment adherence among patients with diabetes (β=0.580, P=0.000).

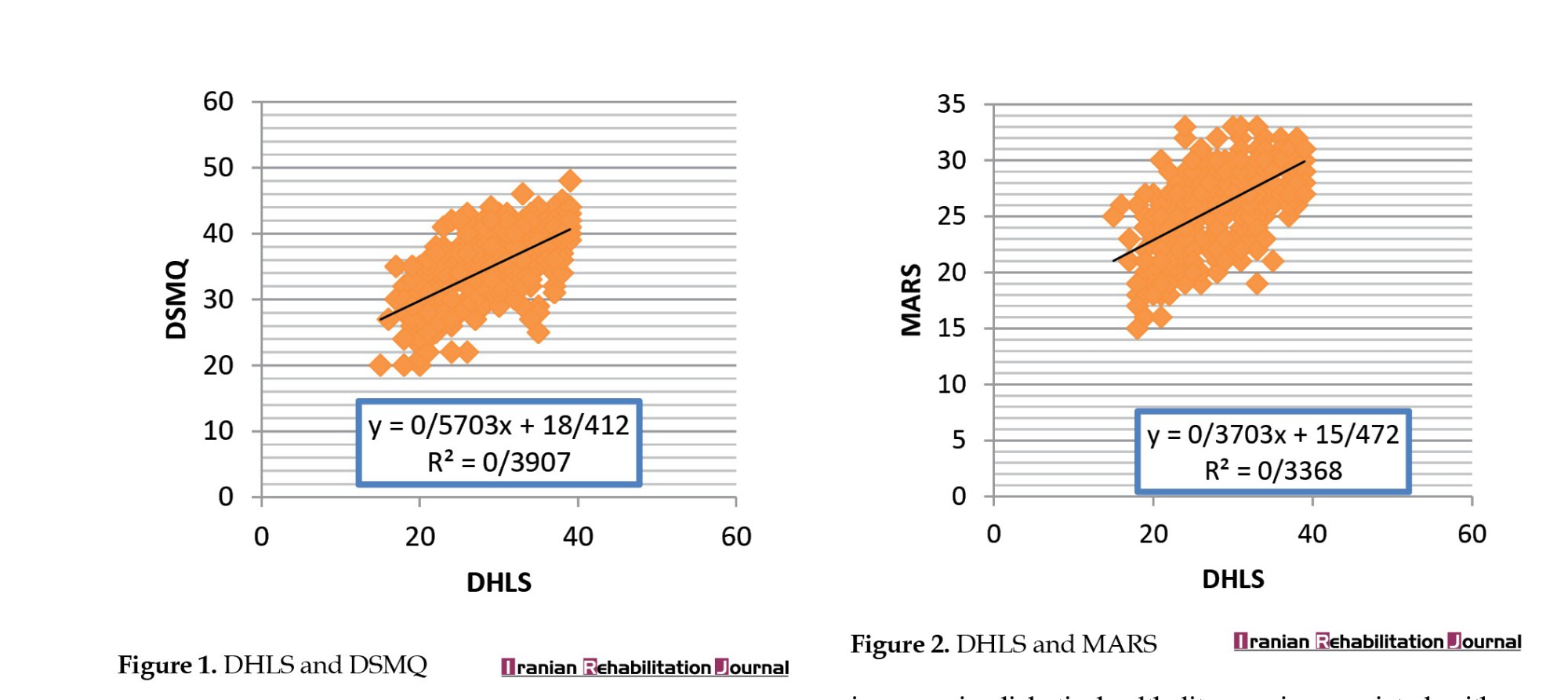
The results depicted in Figure 1 reveal that an increase of 18.412 in diabetic health literacy corresponds to a probability increase of 0.5703 in diabetes self-management. Similarly, Figure 2 demonstrates that a 15.473 point increase in diabetic health literacy is associated with a 0.3703 point increase in diabetes treatment adherence.
Discussion
The results of this examination indicated that 63.1% of the participants reported a slight stage of diabetic self-management, with a median rating of 34.44±5.347. This percentage is better than the findings of a study conducted in Ethiopia, wherein only 84% of patients with diabetes had an insufficient level of self-management. This disparity can be attributed to variations in the accessibility and effectiveness of instructional packages aimed at promoting self-management practices in diabetic patients. According to a study conducted in the same vicinity, structured diabetes education packages significantly improved self-management behaviors among patients with diabetes [5]. The availability of such programs in our vicinity may have contributed to the lower fees of mild self-management. Conversely, the share of patients with diabetes in this study displaying a slight level of self-management is lower than that reported in Italy, where 79.5% of patients achieved this level [18, 19]. One feasible explanation for this discrepancy is the effect of socioeconomic factors, as highlighted by a review of equal regions offering people with disabilities, which noted that higher levels of profit and training are associated with better self-management outcomes [20]. In comparison, the population in our study may face economic or educational challenges that restrict their potential to completely adhere to gold-standard self-management practices.
In terms of treatment adherence, 58.8% of patients with diabetes in this study showed strict adherence to their prescribed routine, with a mean score of 25.87±3.357. This percentage exceeds the results from Kenyatta National Hospital, where only 28.3% of patients with diabetes showed correct adherence. The higher adherence rate found in our study could be attributed to strong communication between healthcare providers and patients. A study from Thailand also confirmed the role of effective counseling in improving adherence among patients with diabetes [21]. In addition, cultural attitudes toward health and treatment compliance in our region may significantly influence adherence behaviors. In contrast, the adherence rate in this study is lower than that documented in Riyadh, Saudi Arabia, where 80.5% of patients with diabetes reported good adherence. This difference may also stem from differences in healthcare systems and patient assistance services. For example, a study in the same region reported that comprehensive follow-up and reminders significantly improved adherence rates [9].
The results revealed that 64.3% of patients with diabetes demonstrated a mild level of health literacy, with an average rating of 28.12±5.861. These results are better than those reported in a study conducted in Malaysia, where only 35% of patients with diabetes showed moderate health literacy. This disparity can be attributed to differences in healthcare infrastructure, admission to education, and public interest campaigns in the studied region compared to Malaysia [22]. In addition, cultural elements and differences in the availability of diabetes training programs may have contributed to this disparity. In our context, local health projects specializing in diabetes management and training may have played a significant role in improving patients’ experiences with their condition. Conversely, our findings are lower than those reported at the University of Hawaii at Manoa, Honolulu, USA, where 55% of patients with diabetes had a moderate degree of health literacy [23]. This difference may be due to more robust national health literacy programs, greater access to health management services, and higher levels of standard education in the USA. Socioeconomic factors, including income and employment costs, may also provide more supportive environments for individuals with diabetes to gain the expertise and skills necessary for effectively managing their condition. Conversely, constraints including limited resources, language differences, and inequalities in access to health management may have hindered our members’ ability to achieve higher levels of health literacy.
The results of the simple linear regression test indicated a significant relationship between health literacy, diabetes self-management, and treatment adherence among patients with diabetes. Health literacy was a strong predictor of diabetes self-management (β=0.625, P<0.001) and adherence to treatment (β=0.580, P<0.001). These findings suggest that promoting health literacy among people with diabetes can significantly improve patients’ ability to effectively manage the disease and adhere to treatment protocols.
Health literacy, defined as the ability to obtain, process, and understand basic health information, plays a crucial role in managing chronic diseases. Studies have consistently shown that individuals with high health literacy have better health outcomes. For example, a systematic review reported that adequate health literacy is associated with improved medication adherence, effective self-management behaviors, and better illness literacy [24]. Likewise, it has been highlighted that limited health literacy in people with diabetes is closely associated with poor blood sugar management and a higher risk of complications [25].
In this study, the regression coefficients provided quantitative evidence of the effect of health literacy on diabetes-related outcomes. Figure 1 shows that an 18.412 unit increase in diabetes health literacy predicts a 0.5703 improvement in diabetes self-management. This finding emphasizes the potential of health literacy as a modifiable determinant of self-management behaviors, including blood sugar monitoring, healthy eating, regular physical activity, and medication adherence. Likewise, patients with higher health literacy scores exhibited superior self-management skills, resulting in fewer hospitalizations and an improved quality of life [26].
Moreover, Figure 2 shows a parallel trend, showing that a 15.473 increase in health literacy in patients with diabetes corresponds to a 0.3703 improvement in treatment adherence. Adherence to treatment is vital in diabetes management because it directly affects blood sugar management and reduces the risk of long-term complications. These findings are consistent with evidence from chronic diseases, which suggests that health literacy interventions targeting medication understanding and regimen complexity lead to significantly higher adherence rates [27]. The practical implications of these findings are significant. Given the global prevalence of diabetes, interventions aimed at improving health literacy may have far-reaching benefits. Tailored educational programs, simplified clinical instructions, and interactive tools can empower patients to take an active role in their management, fill literacy gaps, and address adherence barriers. In addition, healthcare providers should prioritize clear communication and assess patients’ health literacy levels during consultations to ensure understanding and effective disease management.
Conclusion
This study highlights the pivotal role of health literacy in improving diabetes management and treatment adherence among patients with diabetes. The results revealed significant differences in self-management, adherence, and health literacy across regions, influenced by socio-economic, cultural, and healthcare system factors. Health literacy has been identified as a strong predictor of improved self-management and adherence, demonstrating its critical impact on diabetes management. Health management systems should prioritize health literacy interventions, including structured educational programs, simplified communication, and support strategies specifically designed to enhance patients’ understanding and management of diabetes.
Study limitation
This study had several limitations, including the use of a convenience sampling method, which may limit the generalizability of the findings to broader populations. In addition, the cross-sectional design limits the ability to infer causality between diabetes health literacy, self-management, and medication adherence. Self-reported data collection methods may lead to response bias, as participants may overestimate their behaviors. Finally, the study was conducted at a single specialist center, which may limit the diversity of patients’ experiences and healthcare contexts. Future research should address these limitations by employing longitudinal designs, diverse sampling methods, and multicenter approaches.
Ethical Considerations
Compliance with ethical guidelines
This study was approved by the Ethics Committee of Al-Furat Al-Awsat Technical University, Babylon, Iraq (Code: 1717, dated 23/10/2024). The Health Authority of Babylon/Babylon Diabetes and Endocrinology Center in Iraq approved all experimental protocols. All guidelines were followed during the data collection.
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
Conceptualization, data analysis and supervision: Mohammed Malih Radhi; Data collection: Shahad Salam Dakhel Alwatify; Investigation and writing: All authors.
Conflict of interest
The authors declared no conflict of interest.
References
Diabetes is one of the health problems affecting the entire world, affecting tens of millions of people and posing major challenges to patients and health management companies [1]. Effective diabetes management requires individuals to have sufficient health literacy, which plays a pivotal role in understanding the disease, managing symptoms, and adhering to treatment regimens [2]. Health literacy is “the ability to acquire, process, and understand basic health facts and services needed to make appropriate health choices” [3]. For patients with diabetes, health literacy extends beyond general knowledge to include unique abilities in self-management and adherence to treatment, which are crucial for maintaining optimal glycemic control [4, 5].
Research has demonstrated that diabetes self-management behaviors, including blood sugar monitoring, diet regulation, and physical activity, are directly influenced by patients’ health literacy levels [6, 7]. Poor health literacy is associated with inadequate understanding of diabetes, suboptimal self-management behaviors, and poor glycemic management [8]. This highlights the need for targeted interventions that enhance health literacy, enabling patients to manage their conditions effectively [9].
Medication adherence is another crucial aspect of diabetes management that greatly intersects with health literacy [10]. Certainly, non-adherence to prescribed medications is an important limitation to achieving favorable therapeutic outcomes in chronic conditions, including diabetes [11]. Patients with low health literacy may also fail to recognize medication instructions, leading to neglected dosing or incorrect administration. This emphasizes the importance of examining how health literacy mediates the relationship between self-management and adherence [12].
Recent studies have begun to highlight the mediating role of health literacy in diabetes outcomes. Health literacy is a crucial mediator, linking diabetes self-management education to improved treatment adherence and medical outcomes. These findings suggest that improving health literacy can not only improve individual health behaviors but also promote better overall management of diabetes, reducing the long-term burden of the disease [13, 14]. Given this context, the current study investigated the mediating role of diabetes health literacy in the relationship between self-management practices and medication adherence among patients with diabetes. Building on previous studies, this study aimed to provide a deeper understanding of the complex relationships between these variables, thus contributing to the development of effective interventions to improve diabetes management outcomes.
Materials and Methods
Study design and sitting
This study used a correlational design to investigate the mediating role of diabetes health literacy in the relationship between self-management practices and medication adherence among patients with diabetes. The design was selected to examine the functional role of diabetes health literacy as a mediator between self-management and adherence behaviors, providing insights into how these variables interact. The studies were conducted at the Babylon Diabetes and Endocrinology Center, a specialized facility providing comprehensive diabetes management. This setting enabled access to various individuals managing diabetes through self-management and prescribed treatment regimens. Patients were managed during their repeated visits to the center, facilitating an efficient record chain.
Study sample
A total of 328 patients with diabetes were recruited using convenience sampling. Participants were approached during their routine visits to the center, ensuring a diverse representation of patients managing their diabetes through self-management and prescribed medication regimens. This study used a convenience sampling method to recruit 328 patients from a target population of 2 262, based on Cochran’s formula for sample size determination. This formula calculates the sample size for large populations and adjusts it for finite populations [15]. The inclusion criteria included individuals aged 18 years or older, with a diagnosis of diabetes of at least six months’ duration, who were able to provide informed consent and respond to study modules. Patients with severe complications or cognitive impairment that could interfere with their ability to participate were excluded. This ensured that the results accurately reflected the relationship between certain study variables.
Study instruments
Data were collected using two validated instruments. The diabetes self-management questionnaire (DSMQ) was used to assess patients’ self-management behaviors, covering aspects, such as glucose management, dietary management, physical activity, and healthcare utilization [16]. The medication adherence report scale (MARS) was used to assess adherence to prescribed medication regimens [17]. The diabetic health literacy scale (DHLS) was used to evaluate the diabetes-related health literacy of patients with diabetes. Both instruments are widely recognized for their reliability and validity in diabetes research.
Validity and reliability
The management fully assessed the validity and reliability of the instruments. Content validity was ensured through expert review, and reliability was tested in a pilot study involving 30 participants. The reliability of the study instruments was assessed using Cronbach’s α and the intraclass correlation coefficient (ICC). Cronbach’s α values exceeded 0.80 for all scales, indicating strong internal consistency. Additionally, ICC was calculated using a two-way mixed-effects model to assess test re-test reliability over a two-week interval. The DSMQ (ICC=0.89), MARS (ICC=0.87), and DHLS (ICC=0.91) demonstrated excellent reliability, confirming the stability and consistency of the measurements over time.
Data collection
Data collection spanned three months, during which participants were provided with questionnaires in a structured interview format. Trained research assistants administered the instruments to minimize response bias and ensure clarity in patient responses. Demographic data, such as age, sex, marital status, education level, occupation, monthly income, and duration of diabetes, were also recorded to support contextual analysis.
Data analysis
The collected data were entered into a statistical program and analyzed using descriptive and inferential statistics. Descriptive statistics, including means, frequencies, and percentages, were used to summarize demographic and clinical variables. The Kolmogorov-Smirnov test (K-S test) was used to test normality. The relationship between diabetes self-management and medication adherence was analyzed using Pearson’s correlation coefficient and simple linear regression. A significance level of P<0.05 was set for all statistical tests.
Results
In terms of statistical frequencies and percentages, Table 1 shows the socio-demographic characteristics of 328 patients who participated in this study. Their ages ranged from 21 to 68 years, with a mean age of 45.35±9.38 years. Notably, more than half of the participants were women (56.1%). The majority (80.2%) were married, (60.4%) were urban residents, (32%) were primary school graduates, (71%) were unemployed, and (38.4%) had a limited or insufficient monthly income. The duration of diabetes ranged from 1 to 28 years, with a mean duration of 9.62±6.477 years.

The results in Table 2 showed that 63.1% of the patients expressed a moderate level of diabetic self-management (34.44±5.347). Regarding treatment adherence, 58.8% of patients with diabetes exhibited good adherence (25.87±3.357). Concerning diabetic health literacy, 46.3% of patients with diabetes had a moderate level (28.12±5.861).

The results of the simple linear regression test in Table 3 indicated that health literacy can serve as a predictor of diabetic self-management (β=0.625, P=0.000) and treatment adherence among patients with diabetes (β=0.580, P=0.000).

The results depicted in Figure 1 reveal that an increase of 18.412 in diabetic health literacy corresponds to a probability increase of 0.5703 in diabetes self-management. Similarly, Figure 2 demonstrates that a 15.473 point increase in diabetic health literacy is associated with a 0.3703 point increase in diabetes treatment adherence.

Discussion
The results of this examination indicated that 63.1% of the participants reported a slight stage of diabetic self-management, with a median rating of 34.44±5.347. This percentage is better than the findings of a study conducted in Ethiopia, wherein only 84% of patients with diabetes had an insufficient level of self-management. This disparity can be attributed to variations in the accessibility and effectiveness of instructional packages aimed at promoting self-management practices in diabetic patients. According to a study conducted in the same vicinity, structured diabetes education packages significantly improved self-management behaviors among patients with diabetes [5]. The availability of such programs in our vicinity may have contributed to the lower fees of mild self-management. Conversely, the share of patients with diabetes in this study displaying a slight level of self-management is lower than that reported in Italy, where 79.5% of patients achieved this level [18, 19]. One feasible explanation for this discrepancy is the effect of socioeconomic factors, as highlighted by a review of equal regions offering people with disabilities, which noted that higher levels of profit and training are associated with better self-management outcomes [20]. In comparison, the population in our study may face economic or educational challenges that restrict their potential to completely adhere to gold-standard self-management practices.
In terms of treatment adherence, 58.8% of patients with diabetes in this study showed strict adherence to their prescribed routine, with a mean score of 25.87±3.357. This percentage exceeds the results from Kenyatta National Hospital, where only 28.3% of patients with diabetes showed correct adherence. The higher adherence rate found in our study could be attributed to strong communication between healthcare providers and patients. A study from Thailand also confirmed the role of effective counseling in improving adherence among patients with diabetes [21]. In addition, cultural attitudes toward health and treatment compliance in our region may significantly influence adherence behaviors. In contrast, the adherence rate in this study is lower than that documented in Riyadh, Saudi Arabia, where 80.5% of patients with diabetes reported good adherence. This difference may also stem from differences in healthcare systems and patient assistance services. For example, a study in the same region reported that comprehensive follow-up and reminders significantly improved adherence rates [9].
The results revealed that 64.3% of patients with diabetes demonstrated a mild level of health literacy, with an average rating of 28.12±5.861. These results are better than those reported in a study conducted in Malaysia, where only 35% of patients with diabetes showed moderate health literacy. This disparity can be attributed to differences in healthcare infrastructure, admission to education, and public interest campaigns in the studied region compared to Malaysia [22]. In addition, cultural elements and differences in the availability of diabetes training programs may have contributed to this disparity. In our context, local health projects specializing in diabetes management and training may have played a significant role in improving patients’ experiences with their condition. Conversely, our findings are lower than those reported at the University of Hawaii at Manoa, Honolulu, USA, where 55% of patients with diabetes had a moderate degree of health literacy [23]. This difference may be due to more robust national health literacy programs, greater access to health management services, and higher levels of standard education in the USA. Socioeconomic factors, including income and employment costs, may also provide more supportive environments for individuals with diabetes to gain the expertise and skills necessary for effectively managing their condition. Conversely, constraints including limited resources, language differences, and inequalities in access to health management may have hindered our members’ ability to achieve higher levels of health literacy.
The results of the simple linear regression test indicated a significant relationship between health literacy, diabetes self-management, and treatment adherence among patients with diabetes. Health literacy was a strong predictor of diabetes self-management (β=0.625, P<0.001) and adherence to treatment (β=0.580, P<0.001). These findings suggest that promoting health literacy among people with diabetes can significantly improve patients’ ability to effectively manage the disease and adhere to treatment protocols.
Health literacy, defined as the ability to obtain, process, and understand basic health information, plays a crucial role in managing chronic diseases. Studies have consistently shown that individuals with high health literacy have better health outcomes. For example, a systematic review reported that adequate health literacy is associated with improved medication adherence, effective self-management behaviors, and better illness literacy [24]. Likewise, it has been highlighted that limited health literacy in people with diabetes is closely associated with poor blood sugar management and a higher risk of complications [25].
In this study, the regression coefficients provided quantitative evidence of the effect of health literacy on diabetes-related outcomes. Figure 1 shows that an 18.412 unit increase in diabetes health literacy predicts a 0.5703 improvement in diabetes self-management. This finding emphasizes the potential of health literacy as a modifiable determinant of self-management behaviors, including blood sugar monitoring, healthy eating, regular physical activity, and medication adherence. Likewise, patients with higher health literacy scores exhibited superior self-management skills, resulting in fewer hospitalizations and an improved quality of life [26].
Moreover, Figure 2 shows a parallel trend, showing that a 15.473 increase in health literacy in patients with diabetes corresponds to a 0.3703 improvement in treatment adherence. Adherence to treatment is vital in diabetes management because it directly affects blood sugar management and reduces the risk of long-term complications. These findings are consistent with evidence from chronic diseases, which suggests that health literacy interventions targeting medication understanding and regimen complexity lead to significantly higher adherence rates [27]. The practical implications of these findings are significant. Given the global prevalence of diabetes, interventions aimed at improving health literacy may have far-reaching benefits. Tailored educational programs, simplified clinical instructions, and interactive tools can empower patients to take an active role in their management, fill literacy gaps, and address adherence barriers. In addition, healthcare providers should prioritize clear communication and assess patients’ health literacy levels during consultations to ensure understanding and effective disease management.
Conclusion
This study highlights the pivotal role of health literacy in improving diabetes management and treatment adherence among patients with diabetes. The results revealed significant differences in self-management, adherence, and health literacy across regions, influenced by socio-economic, cultural, and healthcare system factors. Health literacy has been identified as a strong predictor of improved self-management and adherence, demonstrating its critical impact on diabetes management. Health management systems should prioritize health literacy interventions, including structured educational programs, simplified communication, and support strategies specifically designed to enhance patients’ understanding and management of diabetes.
Study limitation
This study had several limitations, including the use of a convenience sampling method, which may limit the generalizability of the findings to broader populations. In addition, the cross-sectional design limits the ability to infer causality between diabetes health literacy, self-management, and medication adherence. Self-reported data collection methods may lead to response bias, as participants may overestimate their behaviors. Finally, the study was conducted at a single specialist center, which may limit the diversity of patients’ experiences and healthcare contexts. Future research should address these limitations by employing longitudinal designs, diverse sampling methods, and multicenter approaches.
Ethical Considerations
Compliance with ethical guidelines
This study was approved by the Ethics Committee of Al-Furat Al-Awsat Technical University, Babylon, Iraq (Code: 1717, dated 23/10/2024). The Health Authority of Babylon/Babylon Diabetes and Endocrinology Center in Iraq approved all experimental protocols. All guidelines were followed during the data collection.
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
Conceptualization, data analysis and supervision: Mohammed Malih Radhi; Data collection: Shahad Salam Dakhel Alwatify; Investigation and writing: All authors.
Conflict of interest
The authors declared no conflict of interest.
References
- Lovic D, Piperidou A, Zografou I, Grassos H, Pittaras A, Manolis A. The growing epidemic of diabetes mellitus. Current Vascular Pharmacology. 2020; 18(2):104-9. [DOI:10.2174/1570161117666190405165911] [PMID]
- Malih Radhi M, Zair Balat K. Health literacy and its association with medication adherence in patients with hypertension: A mediating role of social support. Iranian Rehabilitation Journal. 2024; 22(1):117-28. [DOI:10.32598/irj.22.1.1989.1]
- Al-Worafi YM. Health literacy and patient education. In: Al-Worafi YM, editor. Handbook of medical and health sciences in developing countries: Education, practice, and research. Cham: Springer International Publishing; 2024. [DOI:10.1007/978-3-030-74786-2_284-1]
- Radhi MM. Degree of disease acceptance and health seeking behaviors for type 2 diabetic patients at Diabetic Center in Hilla City. Medico-Legal Update. 2020; 20(2):853-58. [DOI:10.37506/mlu.v20i2.1347]
- Qassim WJ, Yasir AA, Radhi MM. Assessment of self hardness and its relationship to treatment acceptance for patients with diabetes mellitus at diabetic center in Hilla City/Iraq. Journal of Pharmaceutical Sciences and Research. 2018; 10(1):142-5. [Link]
- Lambrinou E, Hansen TB, Beulens JW. Lifestyle factors, self-management and patient empowerment in diabetes care. European Journal of Preventive Cardiology. 2019; 26(2_suppl):55-63. [DOI:10.1177/2047487319885455] [PMID]
- Zeidi IM, Morshedi H, Alizadeh Otaghvar H. A theory of planned behavior-enhanced intervention to promote health literacy and self-care behaviors of type 2 diabetic patients. Journal of Preventive Medicine and Hygiene. 2021; 61(4):E601-13. [DOI:10.15167/2421-4248/jpmh2020.61.4.1504] [PMID]
- ALSharit BA, Alhalal EA. Effects of health literacy on type 2 diabetic patients' glycemic control, self-management, and quality of life. Saudi Medical Journal. 2022; 43(5):465-72. [DOI:10.15537/smj.2022.43.5.20210917] [PMID]
- Al-Eqabi QA, Niazy SM, Radhi MM. Effectiveness of digital health interventions in managing glycated haemoglobin: A randomized controlled trial. National Journal of Community Medicine. 2024; 15(09):747-53. [DOI:10.55489/njcm.150920244442]
- Malih Radhi M, Niazy SM, Naser Abed S. Individual-related factors associated with treatment adherence among hypertensive patients. Journal of Public Health in Africa. 2023; 14(6):2466. [DOI:10.4081/jphia.2023.2466] [PMID]
- Konstantinou P, Kassianos AP, Georgiou G, Panayides A, Papageorgiou A, Almas I, et al. Barriers, facilitators, and interventions for medication adherence across chronic conditions with the highest non-adherence rates: A scoping review with recommendations for intervention development. Translational Behavioral Medicine. 2020; 10(6):1390-8. [DOI:10.1093/tbm/ibaa118] [PMID]
- Saif S, Bui TTT, Srivastava G, Quintana Y. Evaluation of the design and structure of electronic medication labels to improve patient health knowledge and safety: A systematic review. Systematic Reviews. 2024; 13(1):12. [DOI:10.1186/s13643-023-02413-z] [PMID]
- Cengiz D, Agrali H, Korkmaz F, Akyar I. Mediation role of patient engagement on the association between health literacy and self-care behaviours in individuals with type 2 diabetes. International Journal of Nursing Practice. 2022 ; 28(3):e13051. [DOI:10.1111/ijn.13051] [PMID]
- Ong-Artborirak P, Seangpraw K, Boonyathee S, Auttama N, Winaiprasert P. Health literacy, self-efficacy, self-care behaviors, and glycemic control among older adults with type 2 diabetes mellitus: A cross-sectional study in Thai communities. BMC Geriatrics. 2023; 23(1):297. [DOI:10.1186/s12877-023-04010-0] [PMID]
- Cochran WG. Sampling techniques. New Jersey: Johan Wiley & Sons Inc; 1977. [Link]
- Schmitt A, Gahr A, Hermanns N, Kulzer B, Huber J, Haak T. The diabetes self-management questionnaire (DSMQ): Development and evaluation of an instrument to assess diabetes self-care activities associated with glycaemic control. Health and Quality of Life Outcomes. 2013; 11:138. [DOI:10.1186/1477-7525-11-138] [PMID]
- Alsous M, Alhalaiqa F, Abu Farha R, Abdel Jalil M, McElnay J, Horne R. Reliability and validity of Arabic translation of medication adherence report scale (MARS) and beliefs about medication questionnaire (BMQ)-specific for use in children and their parents. PLoS One. 2017; 12(2):e0171863. [DOI:10.1371/journal.pone.0171863] [PMID]
- Moshki M, Alami A, Zadehahmad Z, Ghelichi-Ghojogh M, Dogonchi M, Jafari A. Psychometric properties of Persian version of diabetes health literacy scale (DHLS) in patients with type 2 diabetes. Diabetology & Metabolic Syndrome. 2022; 14(1):139. [DOI:10.1186/s13098-022-00910-0]
- Ausili D, Rossi E, Rebora P, Luciani M, Tonoli L, Ballerini E, et al. Socio-demographic and clinical determinants of self-care in adults with type 2 diabetes: A multicentre observational study. Acta Diabetologica. 2018; 55(7):691-702. [DOI:10.1007/s00592-018-1135-x] [PMID]
- Malih Radhi M, Juma Elywy G, Abbas Khyoosh Al-Eqabi Q. Burdens among wives of disabled people in the light of some social variables. Iranian Rehabilitation Journal. 2023; 21(3):473-84. [DOI:10.32598/irj.21.3.1765.3]
- Wungrath J, Autorn N. Effectiveness of Line application and telephone-based counseling to improve medication adherence: A randomized control trial study among uncontrolled type 2 diabetes patients. Health Promot Perspect. 2021; 11(4):438-43. [DOI:10.34172/hpp.2021.55] [PMID]
- Abdullah A, Liew SM, Salim H, Ng CJ, Chinna K. Prevalence of limited health literacy among patients with type 2 diabetes mellitus: A systematic review. PLoS One. 2019; 14(5):e0216402. [DOI:10.1371/journal.pone.0216402] [PMID]
- Kostareva U, Albright CL, Berens EM, Polansky P, Kadish DE, Ivanov LL, et al. A multilingual integrative review of health literacy in former soviet :union:, Russian-speaking immigrants. International Journal of Environmental Research and Public Health. 2021; 18(2):657. [DOI:10.3390/ijerph18020657]
- Cabellos-García AC, Martínez-Sabater A, Castro-Sánchez E, Kangasniemi M, Juárez-Vela R, Gea-Caballero V. Relation between health literacy, self-care and adherence to treatment with oral anticoagulants in adults: A narrative systematic review. BMC Public Health. 2018; 18(1):1157. [DOI:10.1186/s12889-018-6070-9] [PMID]
- Guo SH, Hsing HC, Lin JL, Lee CC. Relationships between mobile ehealth literacy, diabetes self-care, and glycemic outcomes in Taiwanese patients with type 2 diabetes: Cross-sectional Study. JMIR mHealth and uHealth. 2021; 9(2):e18404.[DOI:10.2196/18404] [PMID]
- Elywy GJ, Radhi MM, AlEqabi QA. Relationship between social support and self-hardiness among breast cancer women in Nasiriyah, Iraq. Journal of the Pakistan Medical Association. 2023; 73(9):S9-14. [DOI:10.47391/JPMA.IQ-02]
- Radhi MM, Al-Eqabi QA, Hindi NK. Rehabilitation problems of people with motor disabilities at Babylon center for rehabilitation of the disabled. Medical Journal of Babylon. 2023; 20(4):838-43. [DOI:10.4103/MJBL.MJBL_674_23]
Article type: Original Research Articles |
Subject:
Nursing
Received: 2025/01/7 | Accepted: 2025/02/9 | Published: 2025/09/1
Received: 2025/01/7 | Accepted: 2025/02/9 | Published: 2025/09/1
Send email to the article author








