Volume 17, Issue 3 (September 2019)
Iranian Rehabilitation Journal 2019, 17(3): 235-240 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Muhammad Kassim N, Abdullahi A, Usman J S. Relationship Between Psychological Symptoms, Age, Severity of Symptoms, and Societal Integration in Patients With Facial Nerve Paralysis. Iranian Rehabilitation Journal 2019; 17 (3) :235-240
URL: http://irj.uswr.ac.ir/article-1-932-en.html
URL: http://irj.uswr.ac.ir/article-1-932-en.html
1- Department of Physiotherapy, Aminu Kano Teaching Hospital, Kano, Nigeria.
2- Department of Physiotherapy, College of health Science, Bayero University, Kano, Nigeria.
2- Department of Physiotherapy, College of health Science, Bayero University, Kano, Nigeria.
Full-Text [PDF 565 kb]
(1883 Downloads)
| Abstract (HTML) (4040 Views)
Full-Text: (1238 Views)
1. Introduction
The face is an important part of the human body. It helps us to communicate to the outside world and expresses all our emotions and social and psychological functions [1, 2]. Through these emotions and functions, others can understand our intentions and behaviors. Also, people can recognize others through their facial appearances. Consequently, our faces look is associated with both how we value ourselves, and how people may perceive us. However, Facial Nerve Palsy (FNP) could affect the appearance of the face [3], and lead to psychological, social, and emotional disturbances in the patients. FNP affects the seventh Cranial Nerve (CN VII) known as facial nerve that innervates the muscles of the face, which enables voluntary and involuntary contractions of each side of the face [3, 4]. Injury to this nerve can paralyze the muscles it supplies. The most common cause of this paralysis is Bell’s palsy [5], and the prevalence of FNP is 20 to 30 per 100000 people [6].
Impairment in function or structure of someone’s face can result in lower social participation that be further confounded by environmental and personal factors The International Classification of Functioning (ICF), Disability, and Health) [7]. Similarly, the deformation of the face after FNP may tend to interfere with the affected person’s activities of daily living and social participation, leading to emotional and psychological disturbances [8-10]. Therefore, this study aimed to determine the relationship between psychological symptoms, age, the severity of symptoms, and societal integration in patients with FNP.
2. Methods
Study design
The present study had a cross-sectional design conducting on patients with FNP. The research ethics committees of Kano State Ministry of Health and Aminu Kano teaching Hospital approved this research.
Study participants
The study participants were patients diagnosed with FNP, who were receiving treatment at the outpatient units of physiotherapy departments at Aminu Kano Teaching Hospital, Murtala Muhammad Specialist Hospital, and Muhammad Abdullahi Wase Specialist Hospital in Kano metropolis. The participants were recruited, using purposive sampling technique. The inclusion criteria included patients with unilateral FNP, who were ≥18 years. The participants would be excluded if they had severe cognitive difficulties (scores ≥24 obtained on Mini-Mental State Examination).
The sample size was 96, calculated, using the formula: n=Z2*p(1-p)/d2. Therefore, n=1.92*0.5(1-0.5)/0.12=3.8428*0.5(0.5)/0.01=3.842*0.25/0.01=96, where p is the proportion or the best guess about the value of the proportion of interest. If no information were known about the p, then, p would be 0.5, d would be the tolerance, i.e. how close the proportion of interest is to the desired estimate (0.1) and Z would be 1.96 when the confidence level is 95%.
Study outcomes
The study instruments were Hospital Anxiety and Depression Scale (HADS) to assess psychological distress, House-Brackmann Scale (HBS) to assess the severity of facial nerve damage, and the Facial Nerve Palsy Integration Register (FAIR) to assess community integration of patients with FNP. The HADS is a 14-item scale that generates ordinal data, in which 7 items relate to anxiety, and the other 7 relate to depression [11]. Each item on the questionnaire is scored from 0 to 3.
A score of 0 to 7 is normal, 8 to 10 is borderline abnormal, and 11 to 12 is abnormal. The HBS is a reliable scale that measures the degree of severity of nerve damage in FNP [12]. It grades facial function from 1 (normal) to 6 (complete paralysis). The scale has good psychometric properties, easy to use, and widely accepted in practice [13]. According to House and Brackmann, the scoring is determined by measuring the upward movement of the mid-portion of the top of the eyebrow and the outward movements of the oral commissure [12]. One point is assigned for every 0.25cm upward motion to a maximum of 1cm. The sum of the scores for each structure gives the total HBS score. The maximum score that can be obtained is 8 if both the eyebrow and oral commissure move the full extent of 1cm.
The FAIR is a questionnaire that assesses the level of societal integration. It was designed by two authors (NMK & AA) and validated by experts in the Physiotherapy Department, Bayero University Kano. The questionnaire has two sections. Section A contains quantitative aspects of social integration with 13 questions scored on a 4-point ordinal scale from 0 to 3. The scoring is as follows: 0 (no integration), 1 to 13 (mild integration), 14 to 26 (moderate integration), and 27 to 39 (high integration). Section B of the questionnaire consists of questions that assess the qualitative aspect of societal integration. All the participants were assessed, using the HADS, HBS, and FAIR.
The participants were recruited between June 8, 2015, and July 24, 2015, and the data were collected between August 5, 2015, and November 23, 2015.
Data analysis
The descriptive statistics of frequency and percentage were used to summarize the demographic data. The Spearman’s rho correlation coefficient was used to determine the relationship between anxiety, depression, age of participants, the severity of symptoms, and social integration. Mann-Whitney U test was used to determine differences between men and women in anxiety, depression, and social integration. All analyses were performed in SPSS V. 16.
3. Results
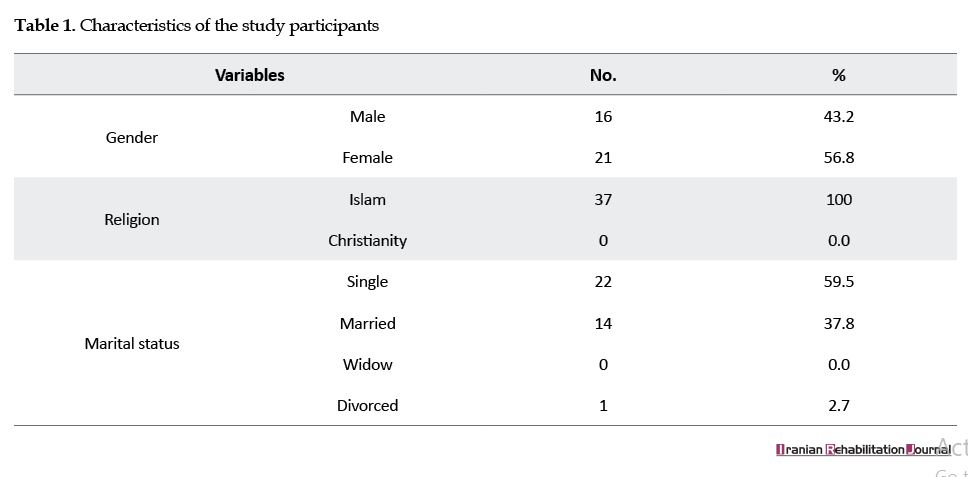
Only 37 participants (16 males and 21 females) with the age range of 14 to 70 years (out of the calculated sample size of 96) took part in the study. (Table 1) presents the details of the participants’ characteristics.
The face is an important part of the human body. It helps us to communicate to the outside world and expresses all our emotions and social and psychological functions [1, 2]. Through these emotions and functions, others can understand our intentions and behaviors. Also, people can recognize others through their facial appearances. Consequently, our faces look is associated with both how we value ourselves, and how people may perceive us. However, Facial Nerve Palsy (FNP) could affect the appearance of the face [3], and lead to psychological, social, and emotional disturbances in the patients. FNP affects the seventh Cranial Nerve (CN VII) known as facial nerve that innervates the muscles of the face, which enables voluntary and involuntary contractions of each side of the face [3, 4]. Injury to this nerve can paralyze the muscles it supplies. The most common cause of this paralysis is Bell’s palsy [5], and the prevalence of FNP is 20 to 30 per 100000 people [6].
Impairment in function or structure of someone’s face can result in lower social participation that be further confounded by environmental and personal factors The International Classification of Functioning (ICF), Disability, and Health) [7]. Similarly, the deformation of the face after FNP may tend to interfere with the affected person’s activities of daily living and social participation, leading to emotional and psychological disturbances [8-10]. Therefore, this study aimed to determine the relationship between psychological symptoms, age, the severity of symptoms, and societal integration in patients with FNP.
2. Methods
Study design
The present study had a cross-sectional design conducting on patients with FNP. The research ethics committees of Kano State Ministry of Health and Aminu Kano teaching Hospital approved this research.
Study participants
The study participants were patients diagnosed with FNP, who were receiving treatment at the outpatient units of physiotherapy departments at Aminu Kano Teaching Hospital, Murtala Muhammad Specialist Hospital, and Muhammad Abdullahi Wase Specialist Hospital in Kano metropolis. The participants were recruited, using purposive sampling technique. The inclusion criteria included patients with unilateral FNP, who were ≥18 years. The participants would be excluded if they had severe cognitive difficulties (scores ≥24 obtained on Mini-Mental State Examination).
The sample size was 96, calculated, using the formula: n=Z2*p(1-p)/d2. Therefore, n=1.92*0.5(1-0.5)/0.12=3.8428*0.5(0.5)/0.01=3.842*0.25/0.01=96, where p is the proportion or the best guess about the value of the proportion of interest. If no information were known about the p, then, p would be 0.5, d would be the tolerance, i.e. how close the proportion of interest is to the desired estimate (0.1) and Z would be 1.96 when the confidence level is 95%.
Study outcomes
The study instruments were Hospital Anxiety and Depression Scale (HADS) to assess psychological distress, House-Brackmann Scale (HBS) to assess the severity of facial nerve damage, and the Facial Nerve Palsy Integration Register (FAIR) to assess community integration of patients with FNP. The HADS is a 14-item scale that generates ordinal data, in which 7 items relate to anxiety, and the other 7 relate to depression [11]. Each item on the questionnaire is scored from 0 to 3.
A score of 0 to 7 is normal, 8 to 10 is borderline abnormal, and 11 to 12 is abnormal. The HBS is a reliable scale that measures the degree of severity of nerve damage in FNP [12]. It grades facial function from 1 (normal) to 6 (complete paralysis). The scale has good psychometric properties, easy to use, and widely accepted in practice [13]. According to House and Brackmann, the scoring is determined by measuring the upward movement of the mid-portion of the top of the eyebrow and the outward movements of the oral commissure [12]. One point is assigned for every 0.25cm upward motion to a maximum of 1cm. The sum of the scores for each structure gives the total HBS score. The maximum score that can be obtained is 8 if both the eyebrow and oral commissure move the full extent of 1cm.
The FAIR is a questionnaire that assesses the level of societal integration. It was designed by two authors (NMK & AA) and validated by experts in the Physiotherapy Department, Bayero University Kano. The questionnaire has two sections. Section A contains quantitative aspects of social integration with 13 questions scored on a 4-point ordinal scale from 0 to 3. The scoring is as follows: 0 (no integration), 1 to 13 (mild integration), 14 to 26 (moderate integration), and 27 to 39 (high integration). Section B of the questionnaire consists of questions that assess the qualitative aspect of societal integration. All the participants were assessed, using the HADS, HBS, and FAIR.
The participants were recruited between June 8, 2015, and July 24, 2015, and the data were collected between August 5, 2015, and November 23, 2015.
Data analysis
The descriptive statistics of frequency and percentage were used to summarize the demographic data. The Spearman’s rho correlation coefficient was used to determine the relationship between anxiety, depression, age of participants, the severity of symptoms, and social integration. Mann-Whitney U test was used to determine differences between men and women in anxiety, depression, and social integration. All analyses were performed in SPSS V. 16.
3. Results
Only 37 participants (16 males and 21 females) with the age range of 14 to 70 years (out of the calculated sample size of 96) took part in the study. (Table 1) presents the details of the participants’ characteristics.
The result of the study showed a weak negative significant correlation between age and integration (P=0.007). There was a weak positive significant correlation (P=0.008) between depression and integration. No significant relationship was observed between integration and anxiety (P=0.171). There was a significant negative relationship between integration and severity of FNP (P=0.05). (Table 2) presents the details of the results.
Furthermore, the result of the study showed a significant gender difference in integration. There was, however, no significant difference between single and married participants (P=0.358). In addition, anxiety did not significantly differ between males and females. Also, there was a significant difference between males and females in depression. (Table 3) presents the details of the results.
4. Discussion
The findings of this study showed differences in societal integration between males and females (in favor of the males); the severity of FNP decreased as societal integration of the patients increased, and as age increased, the societal integration decreased. Additionally, there was no difference in the integration between single and married ones. Furthermore, there was a significant positive correlation between depression and societal integration, but no significant correlation existed between anxiety and societal integration of the patients. Similarly, the study showed a moderate negative significant correlation between the degree of disfigurement (severity) and societal integration of the patients. This finding is in line with the study results of Bogart et al. Their findings showed that the inability to express oneself with the face (and having a facial difference) is particularly stigmatizing. It tempers with the patients’ societal integrations and total isolation in a sample of adults with Moebius syndrome, a rare congenital condition characterized by facial paralysis [14].
The present study also found that males are more liable to become depressed than females. This finding is in contrast with the findings of previous studies, in which they reported that females have more psychological symptoms than males possibly owing to the greater emphasis placed on their appearance by both themselves and the society [15, 16]. The difference between the findings of the present study and those of the former could be attributed to the context of the present study. In the present study, female samples rarely leave the house compared to their male counterparts. Thus, they will be P=0.05 less likely to come across any depressing stimulus. Additionally, the culture seems to offer females special regard to dissipate their emotions. However, in terms of anxiety, there was no significant difference between males and females.
Regarding age and integration, there was a significant negative correlation between the two variables. Cross et al. found a significant negative correlation between levels of distress, which leads to low integration and age in a sample of patients with FNP following acoustic neuroma surgery [17]. This result is in contrast with the finding of this study, where a significant negative correlation exists between age and social integration of the patients. However, the significant negative correlation between age and integration could be because, in old age, people tend to reduce their social participation.
Regarding marital status, there was no significant difference between single and married participants in terms of their integrating into society. This result may be due to the limited number of samples or great support from their family. Sarkisian and Gerstel reported that single individuals have greater involvement with the larger community [18]. However, in the context of this research, factors such as greater values for married people can give them an equal advantage like single people regarding their involvement in community activities. With regard to depression, anxiety, and societal integration, our study found a significant positive correlation between depression and integration of the patients and a negative non-significant correlation between anxiety and integration.
These findings contrast with the findings of other studies, which reported that psychological symptoms hamper with the integration of FNP patients [14, 19-21]. This difference in the findings may be related to the new scale used in measuring the societal integration of FNP patients in our study. Integration is important for the healing process, as psychosocial support can prevent a patient from distress that may slow down the progress of rehabilitation. This study is, however, limited by the different etiologies of FNP in the study participants, since no difference in the outcomes of interest between the different causes was looked at. This limitation may affect the external validity of the study findings.
5. Conclusions
People with nerve palsy, especially the older patients and women, may be more likely to have problems with community integration. As a result, females may be less depressed than males since they have lower social contacts with others than their male counterparts. Thus, it is recommended that the rehabilitation of people with FNP should have a special focus on societal or community reintegration and management of any psychosocial symptoms associated with the condition.
Ethical Considerations
Compliance with ethical guidelines
The study complied with the ethical guidelines of the hospital where the data was collected in terms of maintaining participants’ privacy, seeking their consent and legal framework that enabled (NMK) collected the data.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors' contributions
All authors contributed equally in preparing this article.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
We would like to thank the staff of Aminu Kano Teaching Hospital, Murtala Muhammad Specialist Hospital and Muhammad Abdullahi Wase Specialists Hospital, in Kano metropolis for their help and assistance during the study.
References
The findings of this study showed differences in societal integration between males and females (in favor of the males); the severity of FNP decreased as societal integration of the patients increased, and as age increased, the societal integration decreased. Additionally, there was no difference in the integration between single and married ones. Furthermore, there was a significant positive correlation between depression and societal integration, but no significant correlation existed between anxiety and societal integration of the patients. Similarly, the study showed a moderate negative significant correlation between the degree of disfigurement (severity) and societal integration of the patients. This finding is in line with the study results of Bogart et al. Their findings showed that the inability to express oneself with the face (and having a facial difference) is particularly stigmatizing. It tempers with the patients’ societal integrations and total isolation in a sample of adults with Moebius syndrome, a rare congenital condition characterized by facial paralysis [14].
The present study also found that males are more liable to become depressed than females. This finding is in contrast with the findings of previous studies, in which they reported that females have more psychological symptoms than males possibly owing to the greater emphasis placed on their appearance by both themselves and the society [15, 16]. The difference between the findings of the present study and those of the former could be attributed to the context of the present study. In the present study, female samples rarely leave the house compared to their male counterparts. Thus, they will be P=0.05 less likely to come across any depressing stimulus. Additionally, the culture seems to offer females special regard to dissipate their emotions. However, in terms of anxiety, there was no significant difference between males and females.
Regarding age and integration, there was a significant negative correlation between the two variables. Cross et al. found a significant negative correlation between levels of distress, which leads to low integration and age in a sample of patients with FNP following acoustic neuroma surgery [17]. This result is in contrast with the finding of this study, where a significant negative correlation exists between age and social integration of the patients. However, the significant negative correlation between age and integration could be because, in old age, people tend to reduce their social participation.
Regarding marital status, there was no significant difference between single and married participants in terms of their integrating into society. This result may be due to the limited number of samples or great support from their family. Sarkisian and Gerstel reported that single individuals have greater involvement with the larger community [18]. However, in the context of this research, factors such as greater values for married people can give them an equal advantage like single people regarding their involvement in community activities. With regard to depression, anxiety, and societal integration, our study found a significant positive correlation between depression and integration of the patients and a negative non-significant correlation between anxiety and integration.
These findings contrast with the findings of other studies, which reported that psychological symptoms hamper with the integration of FNP patients [14, 19-21]. This difference in the findings may be related to the new scale used in measuring the societal integration of FNP patients in our study. Integration is important for the healing process, as psychosocial support can prevent a patient from distress that may slow down the progress of rehabilitation. This study is, however, limited by the different etiologies of FNP in the study participants, since no difference in the outcomes of interest between the different causes was looked at. This limitation may affect the external validity of the study findings.
5. Conclusions
People with nerve palsy, especially the older patients and women, may be more likely to have problems with community integration. As a result, females may be less depressed than males since they have lower social contacts with others than their male counterparts. Thus, it is recommended that the rehabilitation of people with FNP should have a special focus on societal or community reintegration and management of any psychosocial symptoms associated with the condition.
Ethical Considerations
Compliance with ethical guidelines
The study complied with the ethical guidelines of the hospital where the data was collected in terms of maintaining participants’ privacy, seeking their consent and legal framework that enabled (NMK) collected the data.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors' contributions
All authors contributed equally in preparing this article.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
We would like to thank the staff of Aminu Kano Teaching Hospital, Murtala Muhammad Specialist Hospital and Muhammad Abdullahi Wase Specialists Hospital, in Kano metropolis for their help and assistance during the study.
References
- Ekman P, Friesen WV. Pictures of facial affect. In: Little AC, Jones BC, DeBruine LM, editors. The Many Faces of Research on Face Perception. Philosophical Transactions of the Royal Society B. California: Consulting Psychological Press; 2011. [DOI:10.1098/rstb.2010.0386] [PMID] [PMCID]
- De Gelder B. Why bodies? Twelve reasons for including bodily expressions in affective neuroscience. Philosophical Transactions of the Royal Society B: Biological Sciences. 2009; 12(364[1535]):3475-84. [DOI:10.1098/rstb.2009.0190] [PMID] [PMCID]
- Aviv JE, Urken ML. Management of the paralyzed face with microneurovascular free muscle transfer. Archives of Otolaryngology–Head & Neck Surgery. 1992; 1(118[9]):909-12.[DOI:10.1001/archotol.1992.01880090025009] [PMID]
- Ljøstad U, Økstad S, Topstad T, Mygland A, Monstad P. Acute peripheral facial palsy in adults. Journal of Neurology. 2005; 252:672-6. [DOI:10.1007/s00415-005-0715-1] [PMID]
- Morgan M, Nathwant D. Facial palsy and infection: The unfolding story. Clinical Infectious Diseases. 1992; 14:(1):263-71. [DOI:10.1093/clinids/14.1.263] [PMID]
- Junior NA, Junior JJJ, Gignon VF, Kitice AT, Prado LSA, Santos VGW, et al. Facial nerve palsy: Incidence of different ethiologies in a tertiary ambulatory. International Archives of Otorhinolaryngology. 2009; 13(2):167-71.
- World Health Organization. International Classification of Functioning (ICF), Disability and Health [Internet]. 2019 [Updated 2019]. Available from: www.who.int/classifications/icf/icf_more/en/
- Fu L, Bundy C, Sadiq SA. Psychological distress in people with disfigurement from facial palsy. Eye (London). 2011; 25(10):1322-6. [DOI:10.1038/eye.2011.158] [PMID] [PMCID]
- Silva MFF, Guedes ZCF, Cunha MC. Psychological aspects associated with peripheral facial paralysis in sequelae stage: Clinical case study. Revista CEFAC. 2013; 15(4):1025-31. [DOI:10.1590/S1516-18462013000400033]
- Huang B, Xu S, Huang G, Zhang M, Wang W. Psychological factors are closely associated with Bell’s palsy: A case control study. Journal of Huazhong University of Science and Technology. 2012; 32(2):272-9. [DOI:10.1007/s11596-012-0048-0] [PMID]
- Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatrica Scandinavica. 1983; 67:361-70. [DOI:10.1111/j.1600-0447.1983.tb09716.x] [PMID]
- House JW, Brackmnn DE. Facial nerve grading system. Otolaryngol Head & Neck Surgery. 1985; 93:146-7. [DOI:10.1177/019459988509300202] [PMID]
- Coulson SE, Croxson GR, Adams RD, O’Dwyer NJ. Reliability of the “Sydney”, “Sunnybrook”, and “House Brackmann” facial grading systems to assess voluntary movement and synkinesis after facial nerve paralysis. Journal of Otolaryngology Head & Neck Surgery. 2005; 132(4):543-9. [DOI:10.1016/j.otohns.2005.01.027] [PMID]
- Bogart KR, Tickle-Degnen L, Joffe M. Social interaction experiences of adults with Moebius syndrome: A focus group. Journal of Health Psychology. 2012; 17(8):1212-22. [DOI:10.1177/1359105311432491] [PMID]
- Kuehner C. Gender differences in unipolar depression: An update of epidemiological findings and possible explanations. Acta Psychiatrica Scandinavica. 2003; 108(3):163-74. [DOI:10.1034/j.1600-0447.2003.00204.x]
- Mcgregor FC. Social, psychological and cultural dimensions of cosmetic and reconstructive plastic surgery. Aesthetic Plastic Surgery. 1989; 13:1-8.
- Cross T, Sheard E, Garrud C, Nikolopoulos P, O’Donoghue GM. Impact of facial paralysis on patients with acoustic neuroma. The Laryngoscope. 2000; 110:1391542. [DOI:10.1097/00005537-200009000-00024] [PMID]
- Sarkisian N, Gerstel N. Does singlehood isolate or integrate? Examining the link between marital status and ties to kin, friends, and neighbors. Journal of Social and Personal Relationship. 2016; 33(3) 361–84. [DOI:10.1177/0265407515597564]
- Rumsey N, Clarke A, White P, Wyn-Williams, Garlick W. Altered body image: Appearance-related concerns of people with visible disfigurement. Journal of Advanced Nursing. 2004; 48:443-53. [DOI:10.1111/j.1365-2648.2004.03227.x] [PMID]
- VanSwearingen JM, Cohn JF, Bajaj-Luthra A. Specific impairment of smiling increases the severity of depressive symptoms in patients with facial neuromuscular disorders. Aesthetic Plastic Surgery. 1999; 23(6):416-23. [DOI:10.1007/s002669900312] [PMID]
- VanSwearingen JM, Cohn JF, Turnbull J, Mrzia T, Johnson P. Psychological distress: Linking impairment with disability in facial neuromotor disorders. Otolaryngology- Head and Neck Surgery. 1998; 118(6):790-6. [DOI:10.1016/S0194-5998(98)70270-0]
Article type: Original Research Articles |
Subject:
Neurorehabilitation
Received: 2018/11/23 | Accepted: 2019/04/13 | Published: 2019/09/1
Received: 2018/11/23 | Accepted: 2019/04/13 | Published: 2019/09/1
Send email to the article author